What to Expect After a One-Day Visit - Week 1 to Week 6

If you completed a One-Day (single-day) TMS course at Inspire - roughly 20 short sessions delivered in one (or two) tightly scheduled days - you’ve taken a fast, physician-supervised step toward change. This week-by-week roadmap explains typical recovery, the symptom signals we watch for, and exactly when to contact the clinic so you get the support you need.
Quick reminder - What Happened That Day
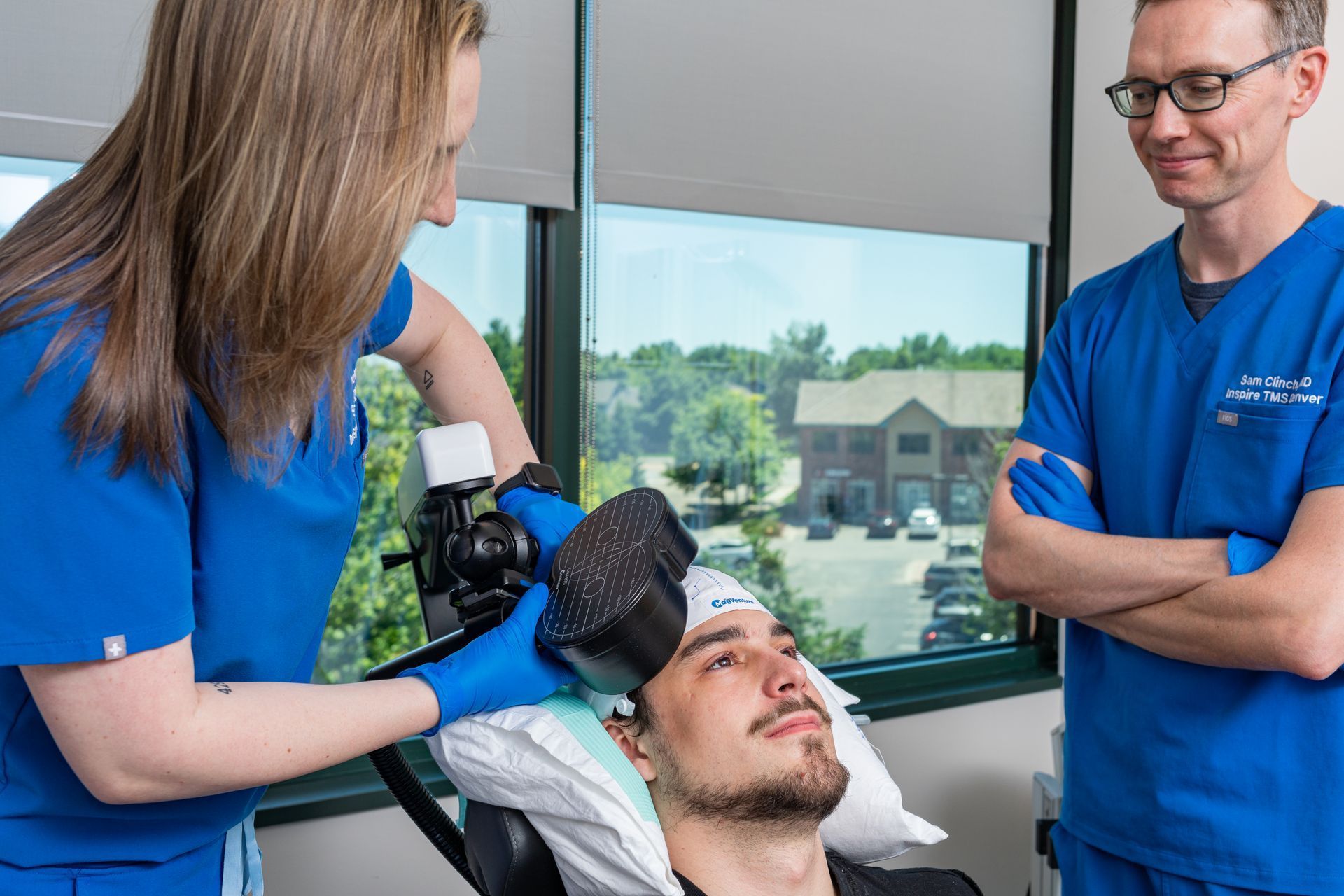
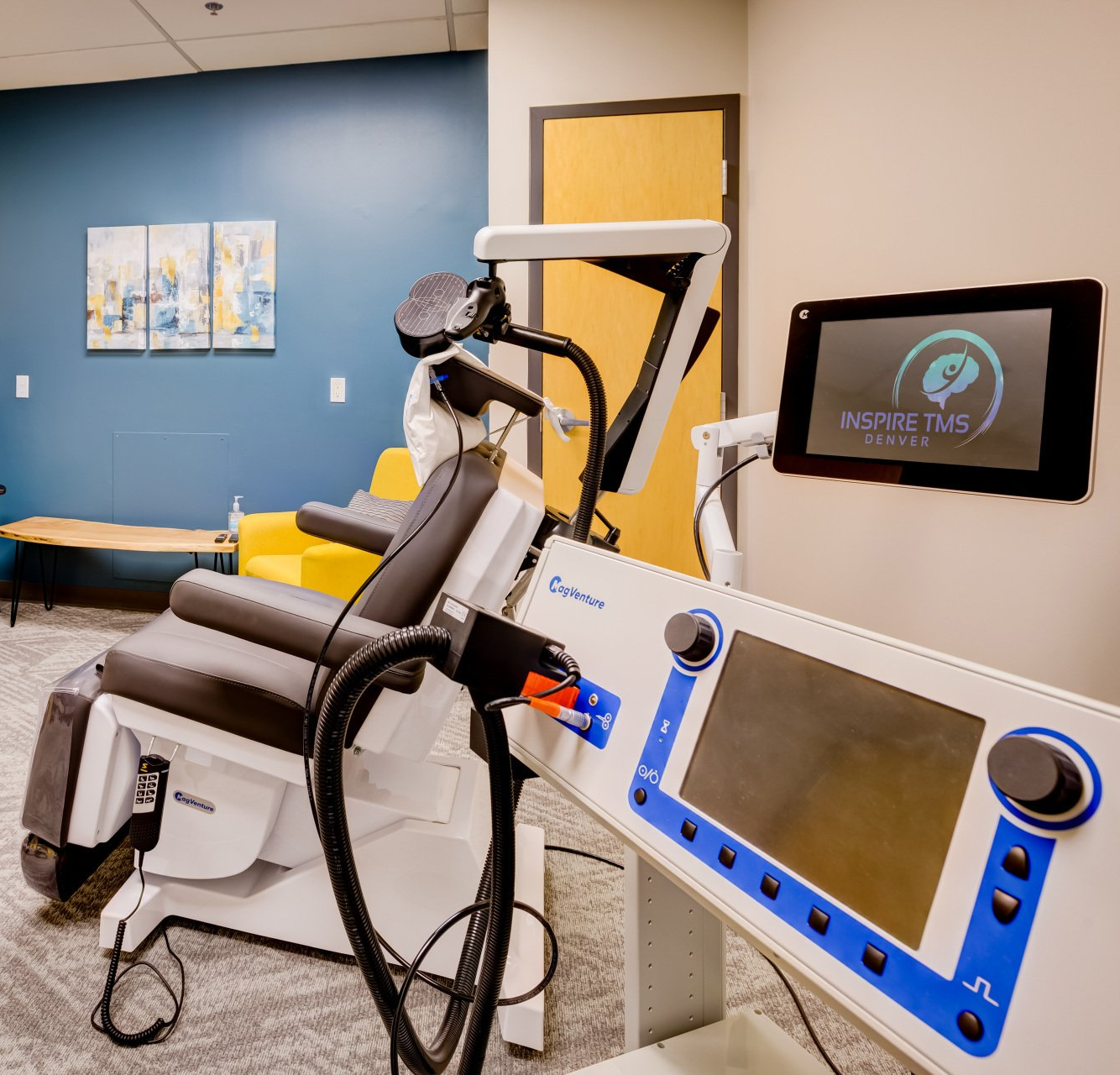
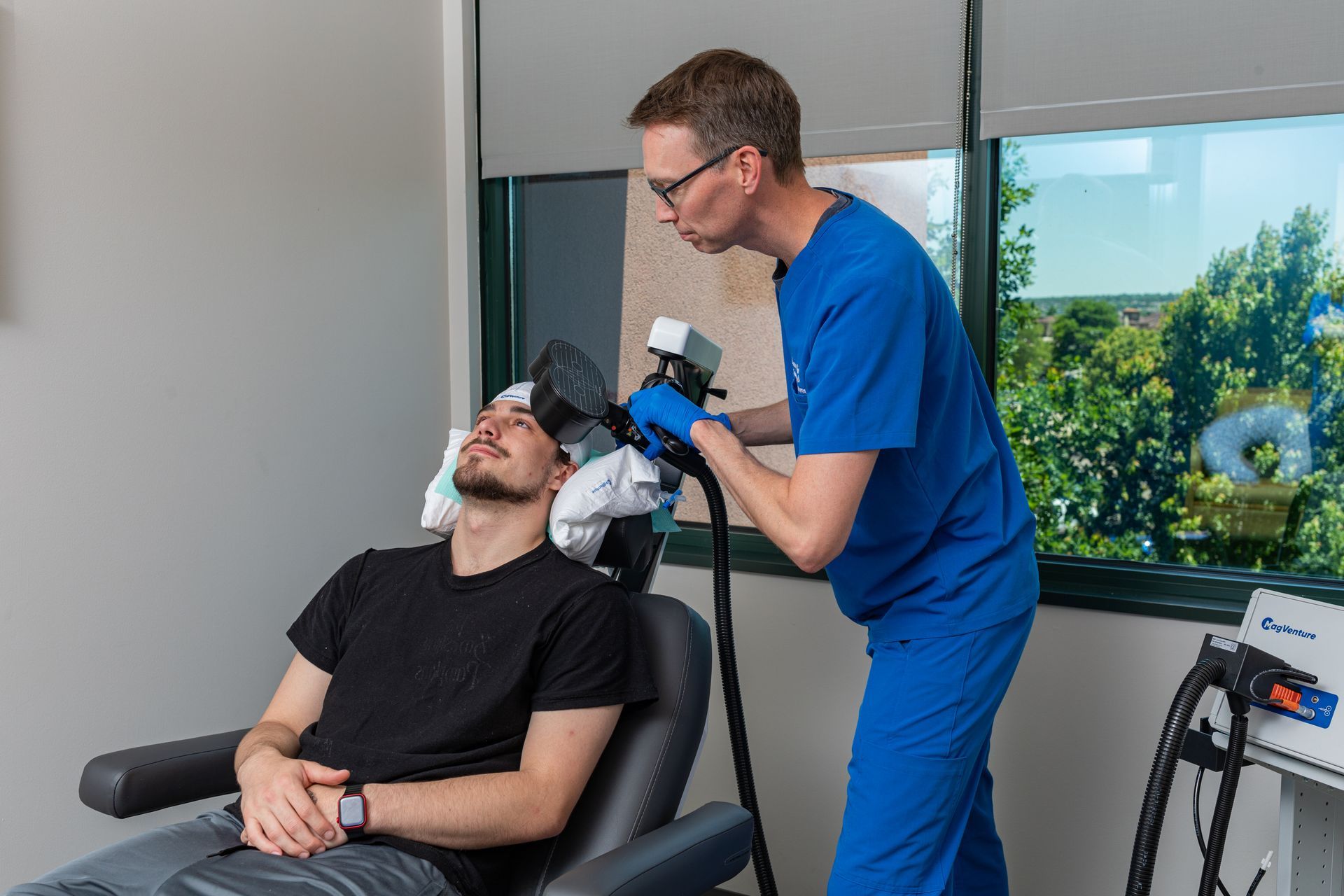
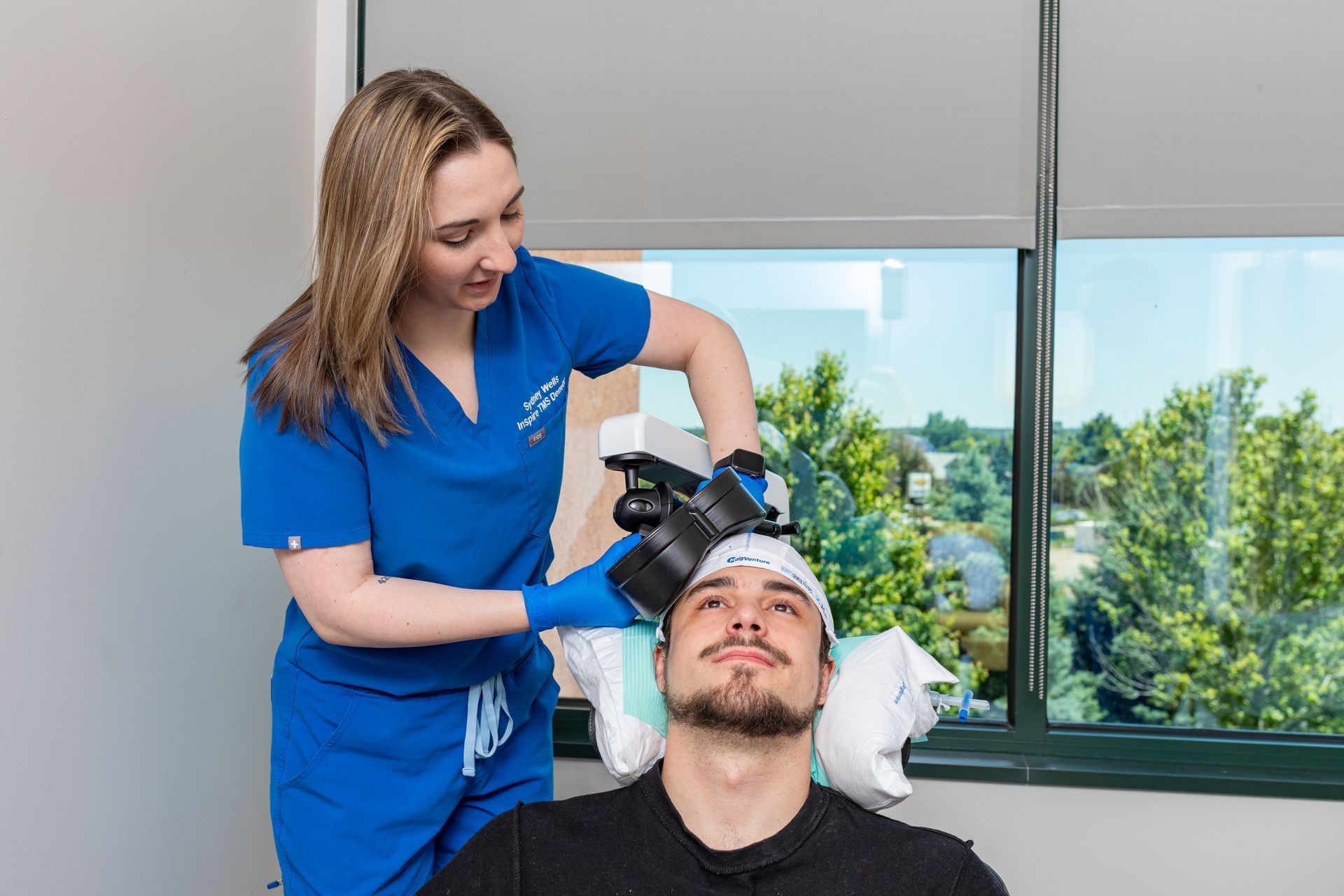
Your One-Day visit began with a physician consult and motor-threshold mapping, so dose and coil position were tailored to your brain. The day was paced with comfort breaks and outcome checks; you left with an end-of-day summary and follow-up plan. That mapping and documentation allow us to make data-driven decisions after you go home.
Week 0 - The Day of Treatment (Immediate Recovery)
Expect: Mild scalp soreness or tapping at the coil site, possible brief headache or fatigue by evening.
Tips: Rest as needed, hydrate, and eat a normal meal. Avoid alcohol for 24 hours. Arrange a ride home if you feel tired.
Call if:
Severe symptoms (worsening headache, confusion, fainting).
Week 1 - First Signals
Expect: Some people notice early changes in sleep, anxiety, or mood; others notice little yet - both are normal. Mild side effects usually resolve.
Clinic check: We compare your Week 1 outcome score to your baseline to assess early improvement.
Call if: Side effects persist or you feel markedly worse.
Read About: Pros & Cons
Week 2 - Emerging Pattern
Expect: Many patients begin to report clearer improvements (more energy, better sleep, less worry); responses vary.
Clinic check: We repeat measures (e.g., PHQ-9) and review meds or sleep if improvement is limited.
Call if: You’re concerned you’re not improving, or side effects interfere with daily life.

Download Your Roadmap to TMS
Want a clear picture of what to expect? Download the TMS Treatment Roadmap by Sydney
Week 3 - Decision Point
Expect: By Week 3 we can often see an early trajectory. Some patients show definite change; others plateau.
Clinic action: If scores stall,
Dr. Clinch may recommend
remapping, pacing changes, or a protocol adjustment - routine, evidence-based steps to improve outcomes.
Call if: Sudden worsening or new neurological symptoms.
Week 4 - Meaningful Improvement Window
Expect: Many responders show substantial improvement by Week 4 (clinically meaningful score drops and better daily functioning).
Clinic action: We review scores and discuss maintenance or next steps. If
you traveled for One-Day, this is a common time to check in with your local provider using the clinician summary we provided.
Weeks 5 - 6 - Consolidation & Next Steps
Expect: Improvements continue for many; others improve after remap or adjustment. By Week 6, we usually have a clear picture: sustained response, partial response needing boosters, or the need for further clinical action.
Clinic action: We plan maintenance (boosters) if helpful, schedule follow-ups, or recommend additional courses as needed.
Practical tips for the first six weeks
- Track sleep & meds. A short diary helps us interpret scores.
- Share your numbers. Small improvements add up - we look at trends, not single scores.
- Keep follow-ups. Don’t skip scheduled checks - they guide timely adjustments.
- Be proactive. Rapid measurement → targeted adjustments → better outcomes.
When to contact Inspire sooner
Call us immediately for: severe/prolonged headache, confusion, fainting, vision changes, or rapidly worsening mood or suicidal thoughts. For non-urgent concerns, reply to your discharge email or call the clinic at (720) 446-8675 during business hours.
Outcomes & follow-up in brief
We use validated scales (PHQ-9, GAD-7, etc.) to quantify change and guide decisions. Typical clinical definitions (like
50% reduction for response) help us set expectations and choose the right next step: remap, adjust, or maintain. Many patients’ reviews that say “life-changing” are backed by measurable score improvements on these tools.
How soon will I notice a benefit?
Some people feel small changes in 1–2 weeks; many see meaningful improvements by weeks 3–4 and consolidation by weeks 4–6. Timelines vary.
What side effects are normal and when should I call?
Mild scalp soreness, brief headache or tiredness are common. Call us for severe/prolonged headache, confusion, fainting, new neurological symptoms, or worsening mood/suicidal thoughts.
Do I need someone to drive me home after ONE-Day?
Many patients can drive the same day, but ONE-Day is intensive and can cause fatigue - arrange a ride if you expect to be tired.
What if my scores haven’t improved by Week 3?
A flat score at Week 3 often prompts a review: mapping, meds, sleep and pacing. We may remap or adjust the protocol - these are standard, evidence-based next steps.

Every Question Answered
Want to know more about TMS? Check out this in-depth guide to TMS therapy with transparent and easy to understand explanations about TMS processes, protocols, and treated conditions.
Latest Posts