Talk to the Doctor
Free 10 Minute Consultation
Free Doctor Call
10–15 Minutes
Free Doctor Call →
10–15 Minutes
Free Doctor Call →
10–15 Minutes
Talk to the Doctor
10–15 Minutes

By Sam Clinch
•
April 13, 2026
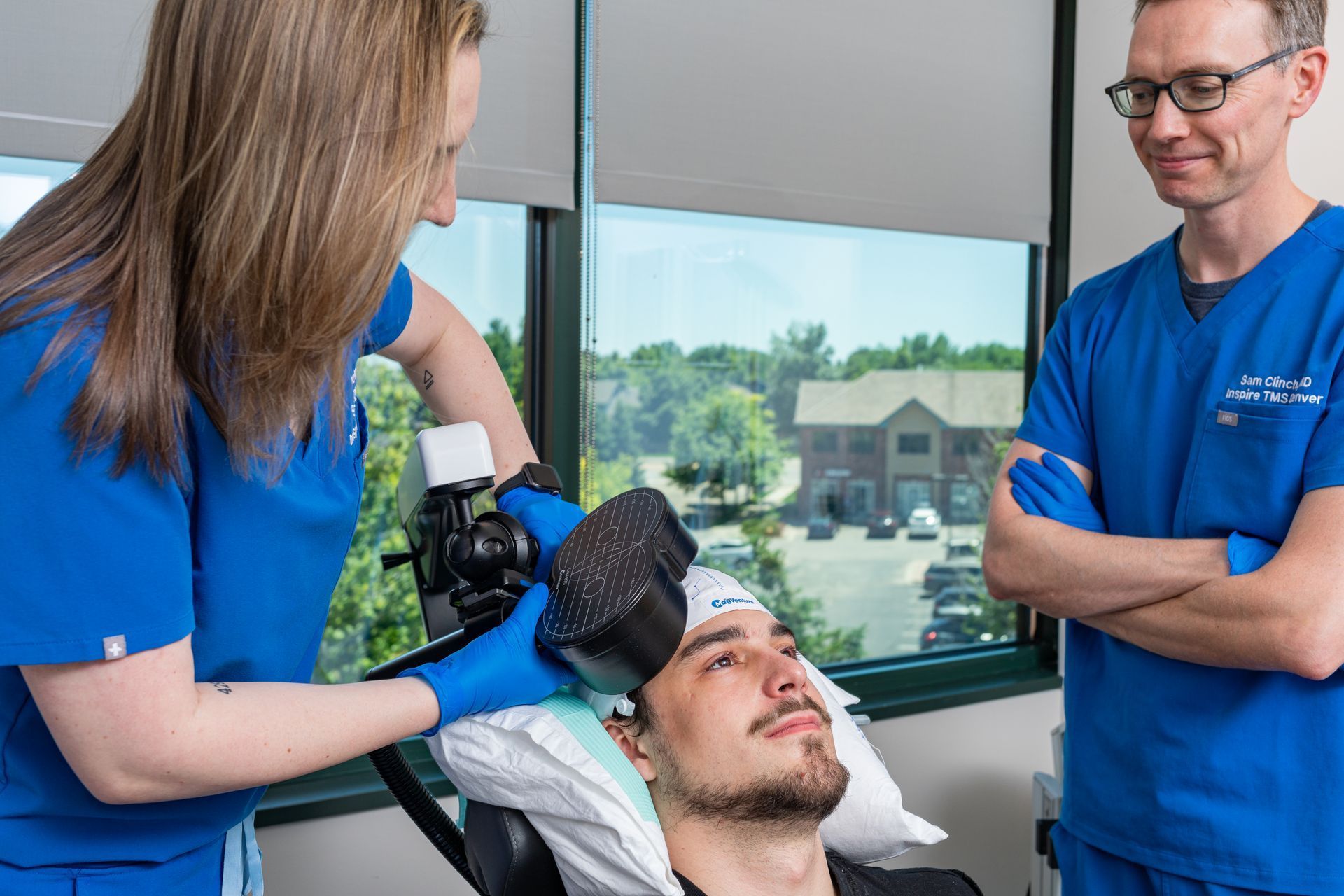
When you’re researching TMS clinics, you’ll see different brand names and device types - MagVenture , NeuroStar, “Deep TMS” (H-coil), and more. That variety can feel confusing, so here’s a plain-language explanation of what the differences mean for you and the smart questions to ask before you book. The short version Device choice mostly affects how stimulation is delivered , which influences: Which protocols a clinic can offer ( standard rTMS , iTBS/Theta Burst, accelerated/One-Day schedules). Session length ( iTBS sessions are very short; older rTMS sessions are longer ). Comfort & noise profile (coil shape and pulse characteristics feel different). Which brain targets are practical (some coils stimulate deeper or wider networks)? Administrative and insurance details (some devices have specific FDA indications or coverage histories). Importantly, good clinical outcomes depend more on clinician skill, mapping, and monitoring than on brand alone. Device capability matters - but physician-led mapping, correct dosing, and careful follow-up make the biggest difference. Device types explained (plain language) Conventional rTMS What it does: Delivers focused stimulation to a relatively small cortical area. Patient experience: Brief tapping sensation at the skull; sessions take longer than iTBS. Why clinics use it: Reliable for many standard depression protocols and widely available. iTBS (intermittent Theta-Burst Stimulation) capable devices What it does: Uses very short bursts of stimulation that produce similar biological effects as standard rTMS but in far less time. Patient experience: Sessions can be minutes long instead of 20–30+ minutes. Why it matters: Shorter appointments are often better for scheduling and comfort; many clinics combine iTBS with accelerated schedules. MagVenture (brand) What it is: A widely used manufacturer; some MagVenture systems are commonly used for accelerated/One-Day regimens. Why you’ll hear it: Clinics sometimes mention MagVenture when they offer compressed/accelerated protocols because of that device’s capabilities in certain settings. NeuroStar (brand) What it is: A long-standing, widely used TMS platform with established clinical workflows and FDA clearances for depression. Why you’ll hear it: NeuroStar has substantial real-world data and brand recognition. Deep TMS / H-coil (different coil geometry) What it does: Designed to stimulate broader or deeper brain regions than a figure-8 coil. Patient experience: Similar sensations but designed for different targets; used for certain FDA-cleared indications (i ncluding OCD in some systems ). Why it matters: May be an option when deeper networks are targeted, depending on diagnosis and evidence.
By Sam Clinch
•
April 13, 2026
If you’ve chosen a ONE-Day (single-day) TMS course - about 20 short sessions delivered in one (or sometimes two) tightly scheduled days - it helps to know exactly how the day will flow. This patient-facing itinerary shows a typical hour-by-hour timeline, what the clinic does between sessions, what to pack, and simple tips to manage fatigue so your visit is as comfortable and effective as possible. You’ll arrive for a physician consult and motor-threshold mapping , then remain at the clinic for a block of short stimulation sessions with scheduled comfort breaks and outcome checks; the clinic monitors you closely and provides an end-of-day review and written summary. Sample hour-by-hour ONE-Day schedule (typical) 08:00 – 09:00 - Arrival, registration & physician consult Check in, confirm meds, and medical history. Short physician discussion about goals and safety. Clinic staff review consent and logistics. 09:00 – 10:00 - Motor-threshold mapping (30–60 min) Mapping identifies the stimulation intensity that produces a small motor response and documents coil coordinates. Staff records the exact coil position (so every session is reproducible). 10:00 – 12:30 - Treatment sessions (Block 1: Sessions 1–10) Multiple short stimulations (each session minutes long; setup/reset time between sessions). Comfort breaks every 2–3 sessions. Nursing/tech staff perform quick symptom checks during breaks. 12:30 – 13:30 - Lunch & outcome check A longer rest; the clinician may perform a short outcome measure (PHQ-9/GAD-7) or check vitals. Time to eat, rest, change clothes if desired, and call for support if needed (ride, family). 13:30 – 17:30 - Treatment sessions (Block 2: Sessions 11–20) Continue with scheduled short sessions and short comfort breaks. The team monitors tolerance, symptom scores, and comfort. If mapping or pacing adjustments are needed, the physician may make micro-changes. 17:30 – 18:00 - End-of-day review & discharge plan Clinician reviews outcome checks, documents the map and dose, and provides a written summary. The team discusses next steps: maintenance, boosters, and scheduling follow-up. Alternative: 1–2 day split - Many patients choose sessions 1–10 on Day 1 and 11–20 on Day 2 to reduce fatigue. The clinic will recommend this based on your history and tolerance. What the clinic does between sessions While you rest, the team is working clinically - not just waiting. Symptom & safety checks: Quick verbal checks, pain comfort ratings, and short outcome items as needed. Documentation: Techs log session parameters, coil coordinates, and any micro-adjustments. Titration µo-adjustments: If a patient reports discomfort or weak responses, the physician may test slight positional or intensity changes. Outcome monitoring: We compare brief score snapshots to baseline to spot early plateau and decide if remapping or pacing changes are required. Support & comfort: Staff provide water, snacks, and a quiet place to rest. They also address anxiety , nausea, or headache immediately.

By Sam Clinch
•
March 31, 2026
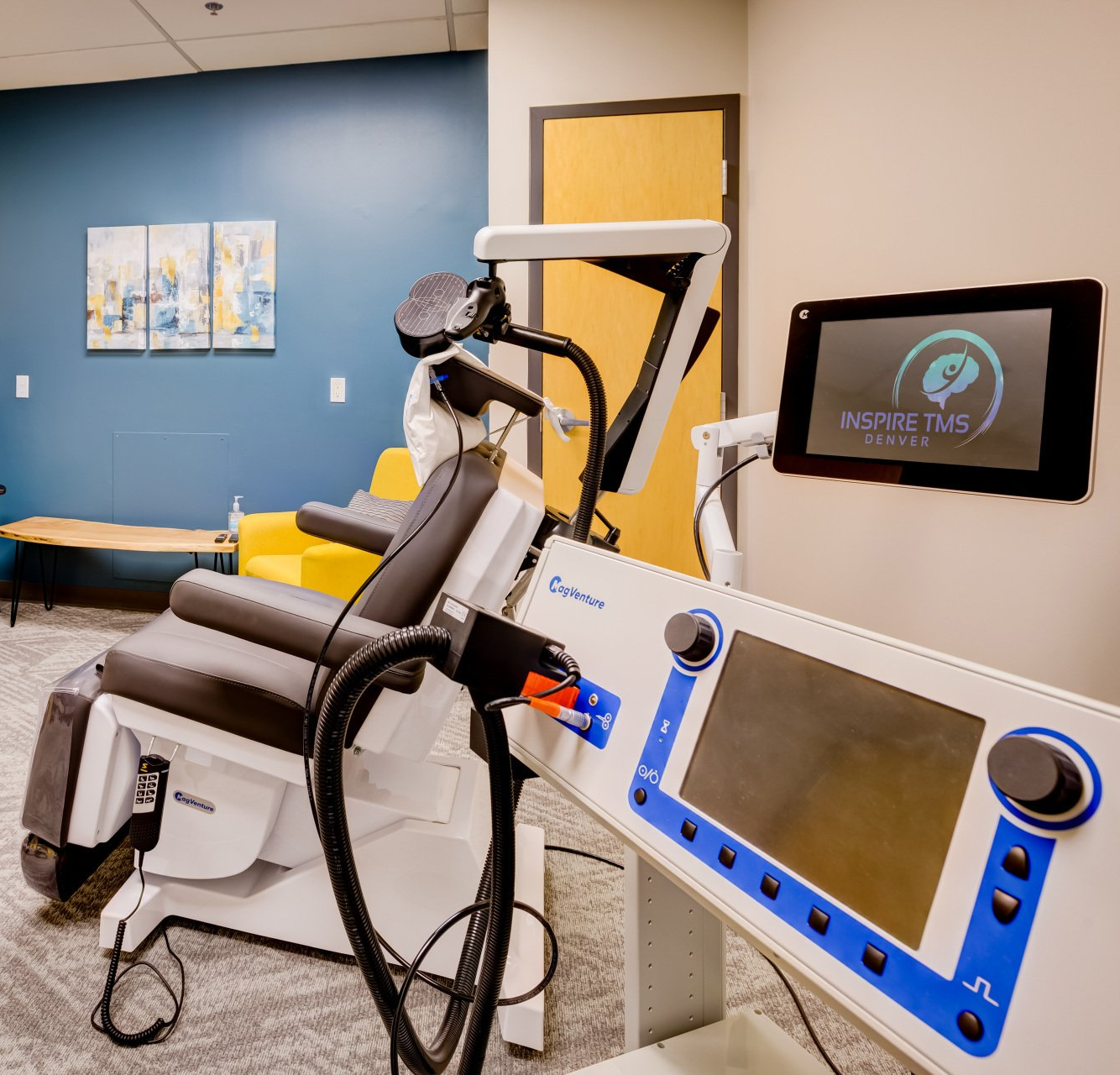
Cost is often the first practical question people ask about One-Day (20-session) and other accelerated TMS options. At Inspire TMS Denver, we treat price transparency as part of clinical care: patients need clear, itemized information to choose the safest, most realistic plan. This guide explains how we build estimates, what coverage looks like for accelerated care, and the payment and financing options we make available. How we build a clear, itemized estimate We prepare estimates the same way we prepare clinical plans - methodically and transparently. An itemized One-Day or accelerated estimate typically lists: Physician consult & safety review (initial consult + med review) Motor-threshold mapping (the clinical calibration before treatment) Treatment sessions (number of sessions, e.g., 20 for a One-Day plan) Monitoring & outcome tracking (score collection, nursing/tech time) Post-treatment follow-up (clinical review, summaries, maintenance planning) Administrative fees (benefits checks, prior authorization support) Any optional items (travel planning support, printed clinician summaries, extra clinician time) We run a benefits check first so the itemized estimate reflects what your insurer will cover and what your likely out-of-pocket responsibility will be. The result is a one-page, line-item document you can use to compare options, plan travel, or request approval from a third party (employer, caregiver, etc.). Typical cost examples & context Costs vary by protocol ( iTBS vs. standard rTMS vs. One-Day) and local pricing. Historically, clinics have published example One-Day packages as a single bundled price; Inspire’s prior examples of accelerated offerings have been in the mid-range of market pricing (clinic examples published previously showed accelerated options around $7,000 versus higher-priced comparators). These are illustrative - we always produce a current, personalized itemized estimate after the benefits check, so you know what applies to your plan. Insurance & coverage realities for accelerated care Standard coverage: Most insurers that cover TMS cover standard, daily courses for treatment-resistant depression when medical criteria are met and prior authorization has been secured. Accelerated/One-Day nuance: True One- Day 20-session packages are often self-pay because many policies don’t yet recognize compressed, single-day regimens as a standard benefit. However, some insurers - and Medicare in certain situations - do cover modified accelerated patterns (for example, two sessions per day) when clinically justified. We run benefits checks to determine exactly how your plan treats accelerated options. Prior authorization & documentation: When coverage is possible, we submit clinical summaries, prior treatment history, and outcome measures to support authorization. Our team helps with appeals if the initial decision is denied. Learn More: Pricing
By Sam Clinch
•
March 30, 2026
The period following completion of an i nitial TMS course is critical . At Inspire TMS Denver , we think of the first 90 days as the window when early gains are consolidated, problems are caught early, and long-term plans (maintenance or boosters) are agreed upon. This practical roadmap explains what clinicians monitor, when a booster or maintenance plan is recommended, and what patients can do to protect and extend benefit. Why the first 90 days matter TMS causes brain-level changes that unfold over weeks . Some people improve quickly and continue to get better; others show delayed responses or need a small clinical adjustment to translate early signals into durable benefit. The first 90 days are when clinicians can: Detect early response vs plateau Make targeted adjustments (remap, pacing, or protocol change) Decide whether boosters or a maintenance schedule will help sustain gains. A proactive, measured approach during this window reduces the chance that patients drift away from care when benefit is still within reach. What clinicians routinely measure and why At Inspire, we rely on objective signals plus clinical judgment. The core things we track are: 1. Standard outcome scores (weekly → monthly) PHQ-9 for depression , GAD-7 for anxiety , and other condition-specific scales. These reveal numeric trends that often precede clear subjective change. We typically collect baseline scores, then repeat them weekly (early weeks), moving to biweekly/monthly checks as things stabilize. 2. Functional markers Sleep, work/school performance, social engagement, and daily activities are measured via short checklists. Function often improves alongside symptom scores - sometimes even earlier. 3. Safety & tolerability Headache, scalp discomfort, fatigue, and any neuro symptoms. Persistent or new neurological issues trigger urgent review. 4. Medication, sleep, and life events Changes in meds, poor sleep, or acute stress/medical events strongly affect response and are always reviewed. 5. Treatment adherence & session data Missed sessions, pacing changes, or protocol deviations are tracked because they affect outcomes.

By Sam Clinch
•
March 30, 2026
If you live in Boulder or the nearby Front Range and are considering TMS , Inspire TMS Denver in Broomfield is an easy, physician-led option for local care and short-trip accelerated plans. Below you’ll find practical local details - approximate drive times, One-Day logistics, hotel & travel tips, and how to get a no-surprise, itemized estimate for your visit. Why Boulder residents come to Inspire TMS Denver Physician-led care: Dr. Samuel Clinch personally oversees mapping and accelerated One-Day courses. Precision mapping: We perform motor-threshold mapping before any accelerated plan so dose and coil position are individualized. One-Day capability: For patients who need fast delivery of the full course, we offer physician-supervised One-Day (20 sessions in 1–2 days) and other accelerated protocols. Outcome tracking & follow-up: We monitor PHQ-9/GAD-7 scores and make data-driven adjustments (remap, pacing, boosters) so your trip produces measurable results.

By Sam Clinch
•
March 30, 2026
Mapping is the clinical step that makes TMS precise. At Inspire TMS Denver, we use motor-threshold mapping to find the coil position and stimulation intensity that reliably affect the brain area we intend to treat. But mapping is not a one-and-done ritual - sometimes a fresh map is the right next step. Remapping is a normal, evidence-based part of precision care: it helps the team fine-tune treatment so sessions are safer, more reproducible, and more likely to work. Below is a clear explanation of why we remap, the remapping process, what patients experience, and real examples of how small changes can produce meaningful clinical gains. Why remap? The clinical reasons We commonly consider remapping after a careful review when any of the following apply: Early plateau or slow progress. If outcome scores (PHQ-9, GAD-7, or other scales) stop improving by the expected window (often around week 3), remapping helps determine whether coil position or intensity is limiting response. Prior TMS elsewhere. If you had TMS with a different device or clinic, anatomical and equipment differences can mean that a new, clinic-specific map improves reproducibility. Medication or medical changes. New medications, dose changes, or medical events that affect cortical excitability can change how your brain responds to stimulation. Change of protocol. Moving from standard rTMS to an accelerated plan, One-Day course, or iTBS may warrant a fresh map to ensure safe and effective dosing. Persistent discomfort or side effects. If you have repeated intolerable scalp discomfort or side effects that suggest coil angle/placement could be optimized, remapping is a logical fix. Equipment or technician change. Different coils or small technique differences can alter the effective stimulation; remapping restores precision. Importantly: remapping is not an admission of failure . It’s a targeted diagnostic step - think of it like recalibrating a medical device to match your brain’s current physiology. What happens during a remap? Comfort: You may feel brief tapping and small muscle twitches during mapping; discomfort is usually minimal. Adjustment period: If we change your dose or target, we monitor closely for comfort and early response. Timeline to effect: A beneficial remap sometimes produces earlier improvement in the following weeks, but improvements still unfold over days to weeks. Documentation: You’ll receive an updated map summary that you can share with other providers.







