Sliding scale pricing for self-pay patients
Meds Didn’t Work.
Therapy Didn’t Work.
TMS Therapy Is Working
• Without Surgery • Without Medication •
• Without Systemic Side Effects
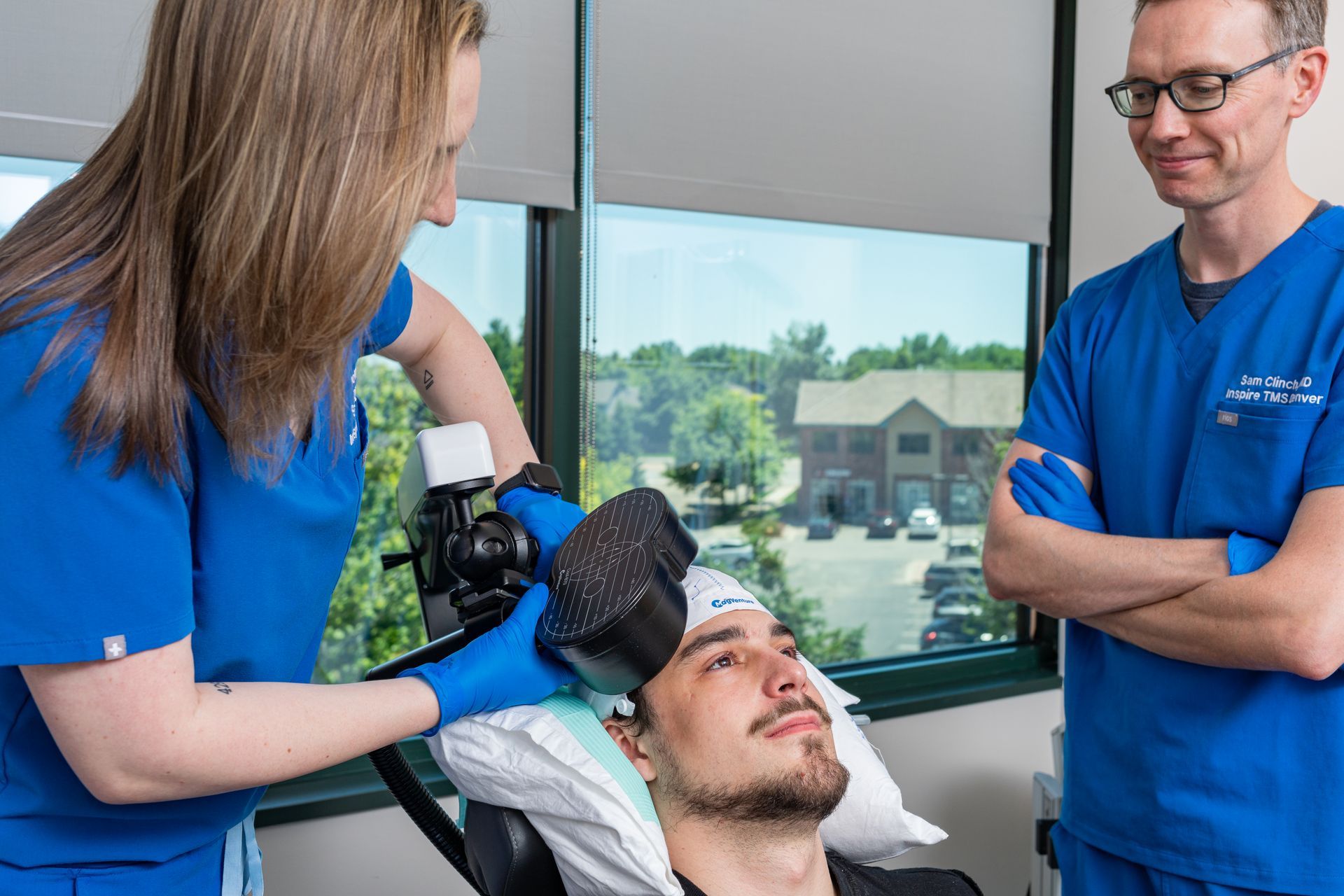
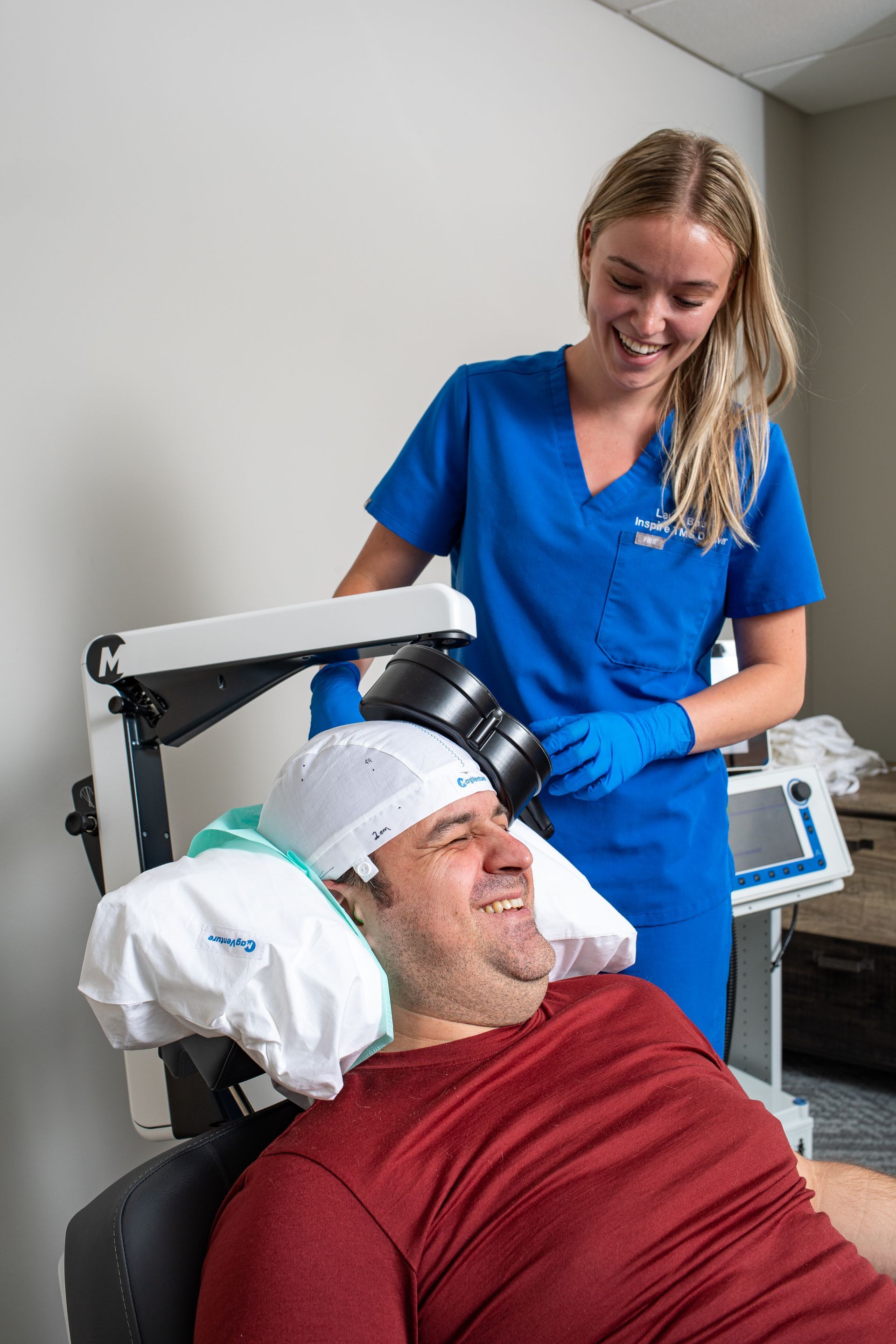
What Is TMS Therapy?
In
30
Seconds

TMS is FDA-approved, drug-free, and effective for depression and other mental health conditions when medications haven’t worked.

No daily meds, no weight gain or other unwanted side effects, no downtime.

Over
15,000 treatments delivered in Denver.
From 8 Weeks to 5 Days
Accelerated TMS for Faster Relief

10 sessions daily over 5 days - condensed protocol, same proven technology and better results

Ideal for busy schedules and for those without close access to a TMS clinic - faster path to relief without medication

All-inclusive rate: $7,500 - includes evaluation, 50 sessions during treatment week, all follow-up visits, and free touch-up sessions within 6 months if needed
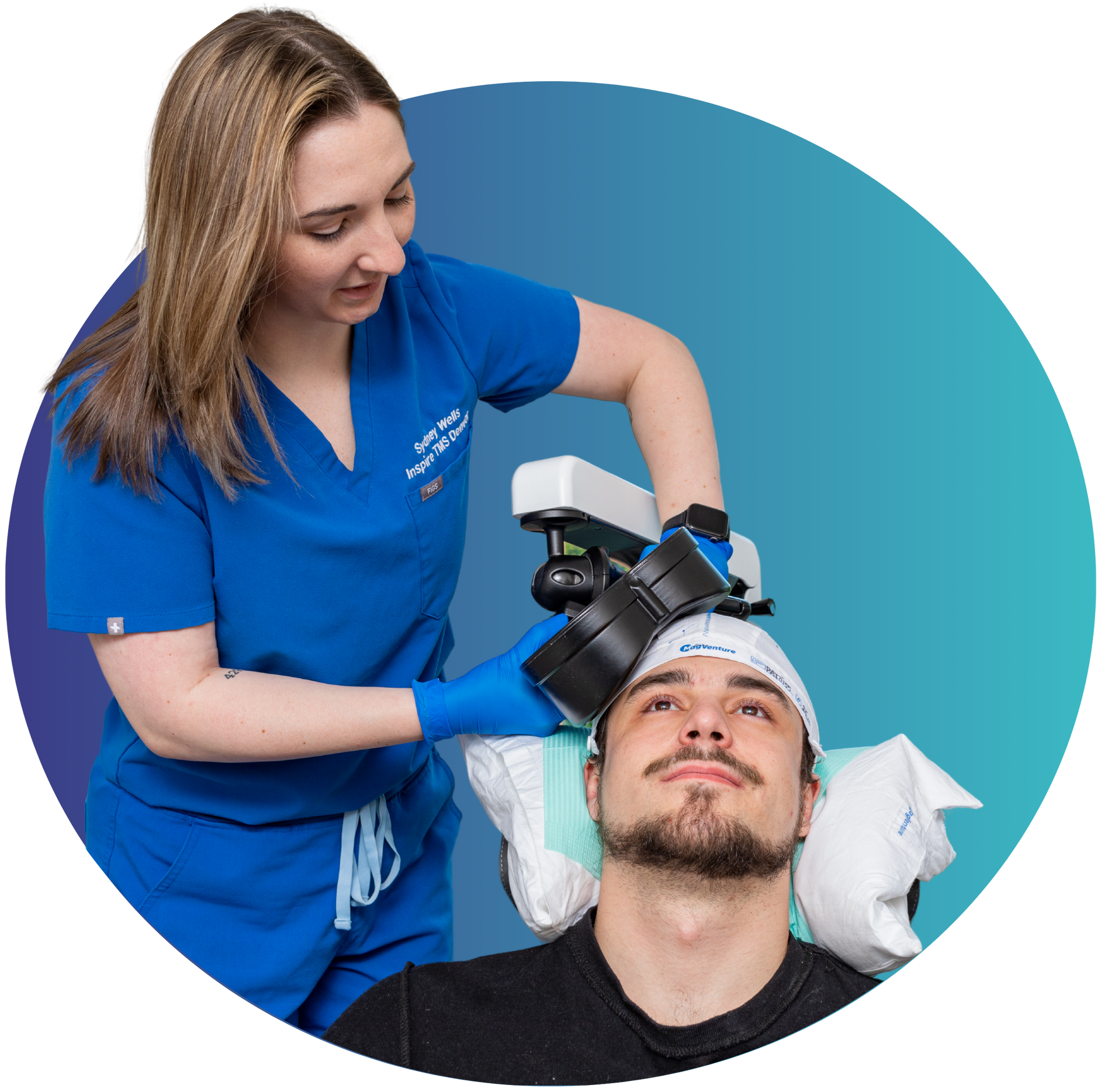
Find the Right TMS Option for You
From first-time treatment to rapid relief, we’re here with a plan that fits.
Non-invasive, FDA-approved treatment for Major Depression & OCD.
Overseen by a psychiatrist and tailored to the needs of younger patients.
Intensive, short-term version delivering 50 sessions over 5 days.
Your
Denver TMS Specialist
Committed to your individual care & recovery

Dr. Samuel Clinch
Your TMS Psychiatrist
Inspire TMS Denver was founded by Sam Clinch, MD, a board-certified Psychiatrist with over 10 years’ experience in the field. He opened Inspire TMS Denver after seeing the limitations of medications and counseling for a significant portion of his patients.

Us vs Them
What sets Inspire TMS apart from typical TMS providers
Inspire TMS Denver
Sliding Scale Pricing Available
5-day Accelerated TMS Protocol
10–15 min call with Doctor
Focused Exclusively on TMS
>80% Clinic Response Rates
Cost Estimator Tool
15,000+ Treatments Completed
Other Clinics
Fixed Pricing Only
Often Unavailable
Long Wait or Intake Staff Only
Larger Multi-Service Clinics
Unpublished or National Data
No estimator or Guidance
Unknown Experience
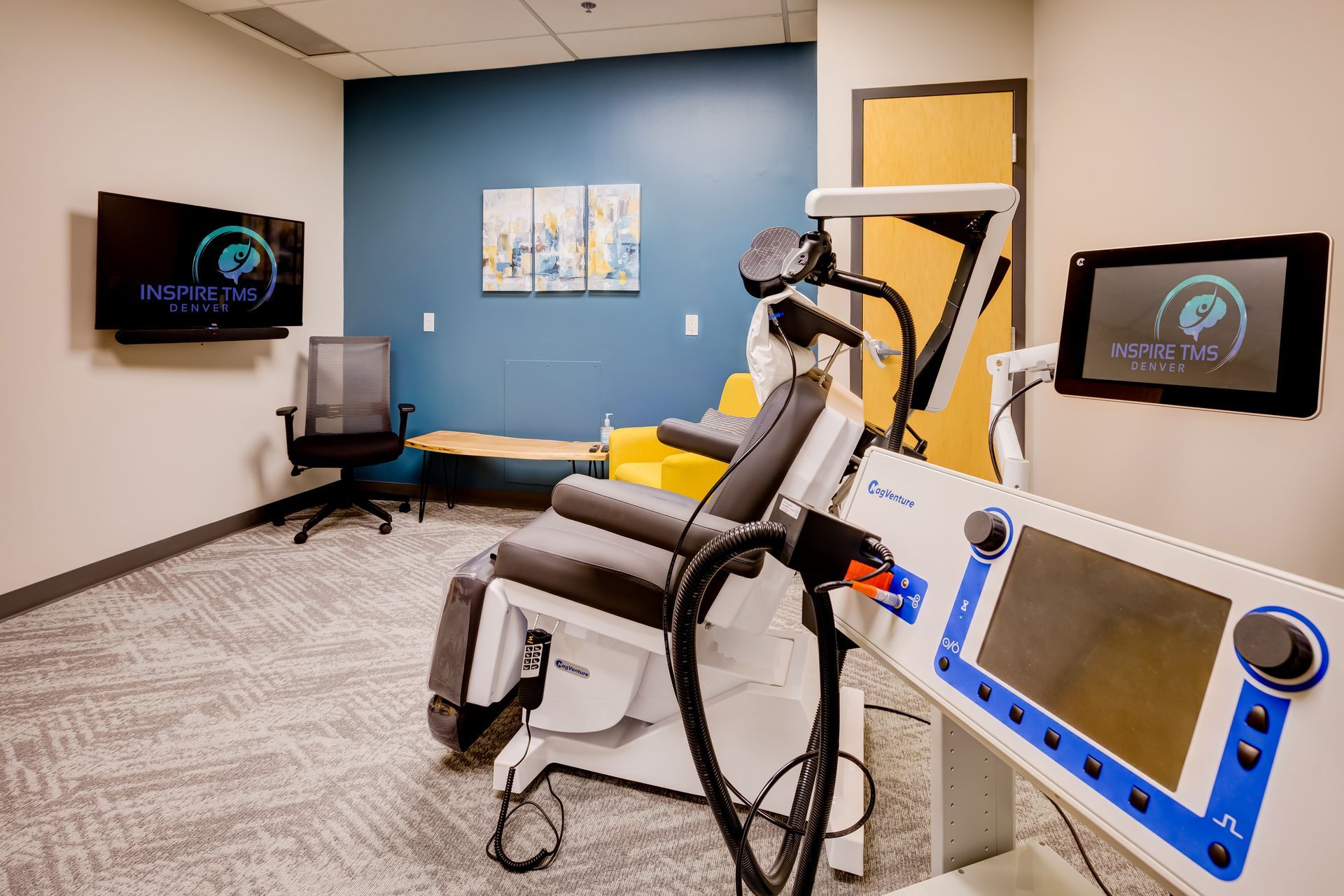
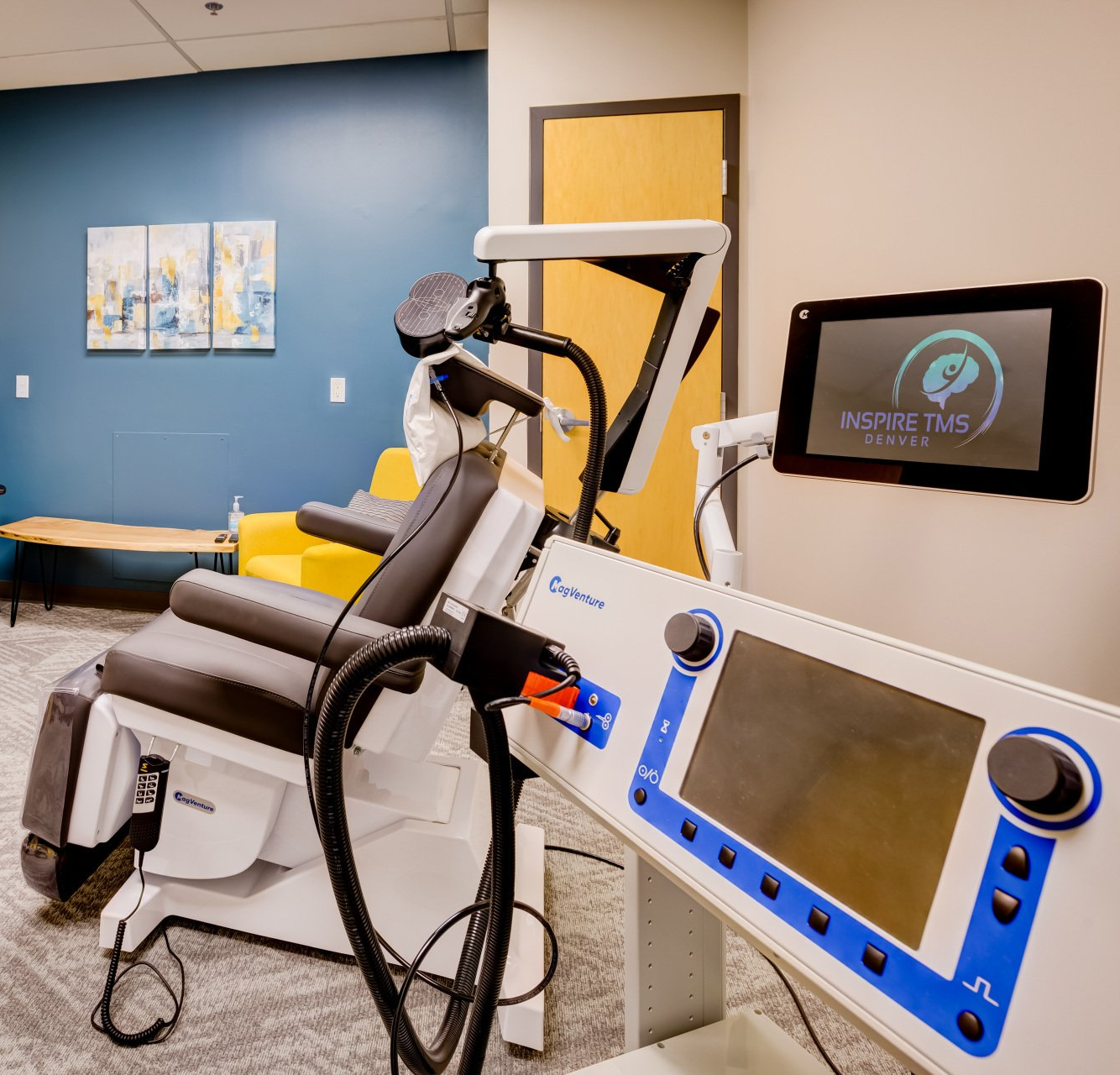
Tour Our Denver Clinic
Walk through our clinic using the arrows below.
TMS Learning Center
Featured Resources

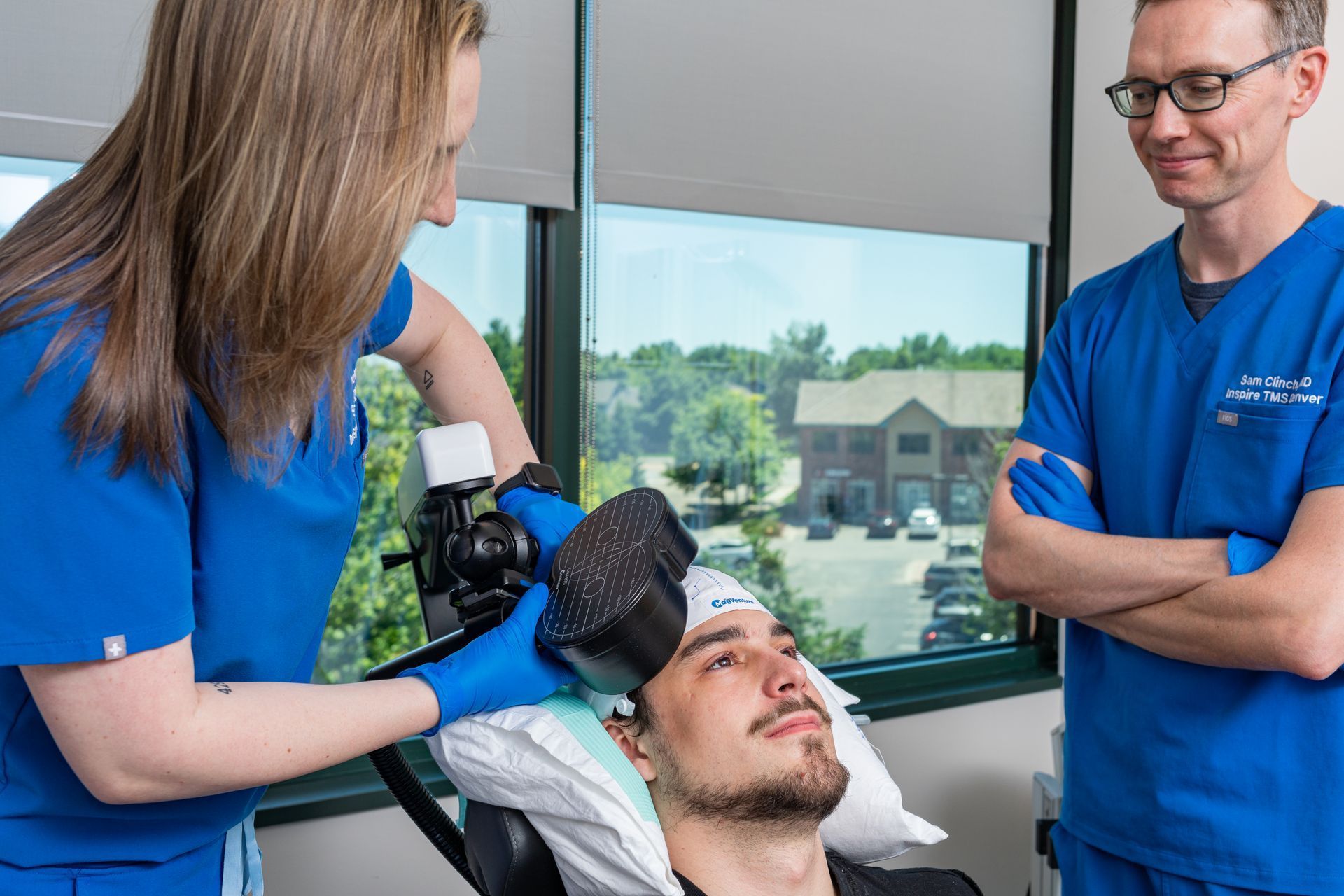




What to Expect With TMS
We make starting TMS simple, supportive, and stress-free. Here’s how it works:
Speak with our psychiatrist or senior team member to explore if TMS is the right fit. Receive a benefits check once providing insurance information. No pressure, no obligation.
Free Doctor Consultation
If eligible, we’ll customize a protocol based on your diagnosis, symptoms, and schedule. Sessions are short and completely non-invasive.
Personalized Treatment Plan
You’ll relax in a comfortable chair while we gently stimulate targeted brain areas using magnetic pulses. No sedation or downtime needed.
Your First Session
TMS is delivered 5 days per week over 6-8 weeks. Accelerated options speed up this time considerably. Our team monitors your progress closely and adjusts care to optimize results.
Ongoing Care & Progress Tracking
Feel the Difference
Most patients notice significant improvements within weeks - with fewer side effects than medication.
Not Sure Where to Start?
Take a quick quiz to get answers about your care options, coverage, and costs - in under 2 minutes.

Is TMS Right for Me?
Find out if TMS is a good fit for your symptoms and treatment history.

Quick 9-question screening

No pressure, no commitment

Personalized feedback

TMS Cost Estimator
Curious about your insurance coverage or out-of-pocket costs?

Coverage check

Self-pay pricing options

Sliding scale

Sliding scale

Talk to a Doctor
Free 10–15 Min Call
Find out if TMS is a good fit for your symptoms and treatment history.

Eligibility & treatment info

Insurance & cost guidance

Personalized care advice
Hear What Our Patients are Saying
40+ Five Star Reviews on TMS Therapy In Denver, Colorado
Making TMS Affordable For Everyone
We believe cost should never be a barrier to effective care. That’s why we offer:


Coverage with all major insurance providers

Easy access to third-party financing options

Free 10–15 minute consultation to get started
Why Choose Inspire TMS Denver
We combine clinical expertise with a personalized, patient-first approach. From board-certified care and flexible pricing to proven treatment outcomes, we’re here to help you find lasting relief - with support every step of the way.

Affordability Made Simple
Insurance, Financing & Sliding Scale Options

Board-Certified Psychiatrist
Over 10 Years of Clinical Experience

Fast-Track TMS Option
Accelerated Protocols for Faster Relief

Proven Patient Outcomes
Success Rates Tracked In-Clinic

Free Doctor Consultation
No Obligation, 10–15 Minute Intro Call

Personalized Care Plans
Tailored TMS Treatment for Every Patient
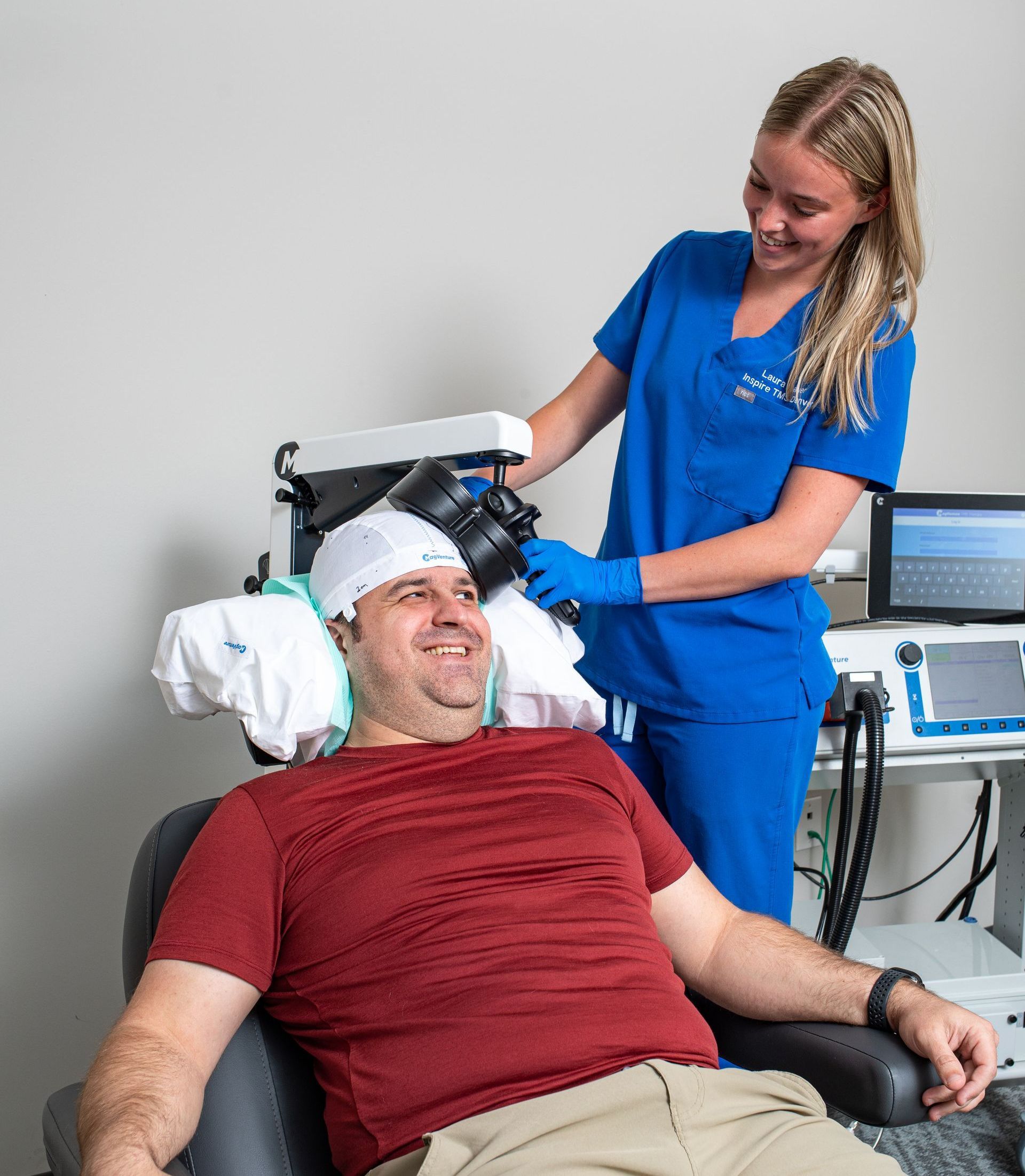
Your Free Consultation
Call us at 720-446-8675 or complete the form below.
Contact Us
We will get back to you as soon as possible.
Please try again later.

What Happens After I Send My Message?

A team member will reach out within one business day

We’ll help you explore if TMS is right for you

You’ll get answers to your questions about treatment, eligibility, and cost