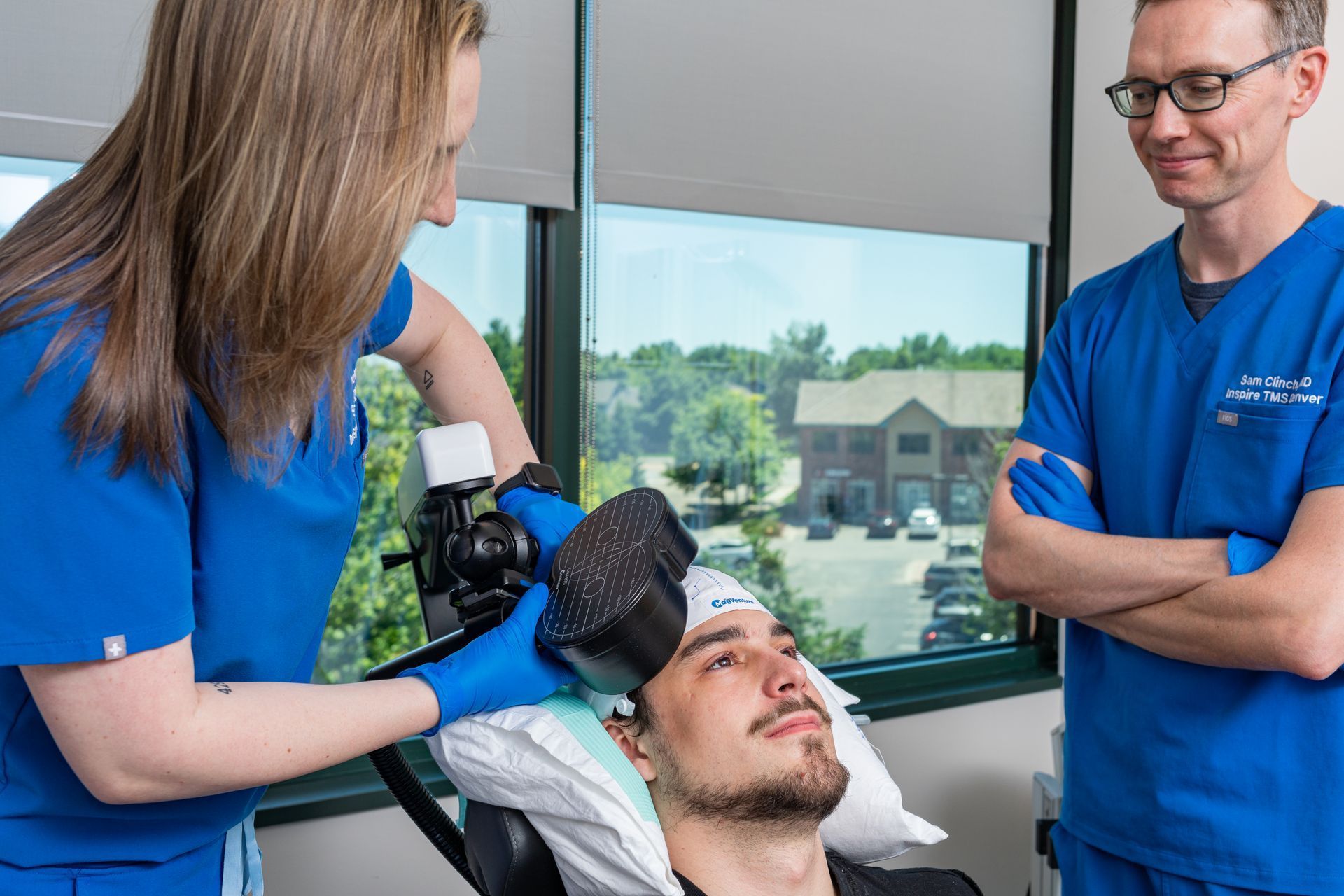
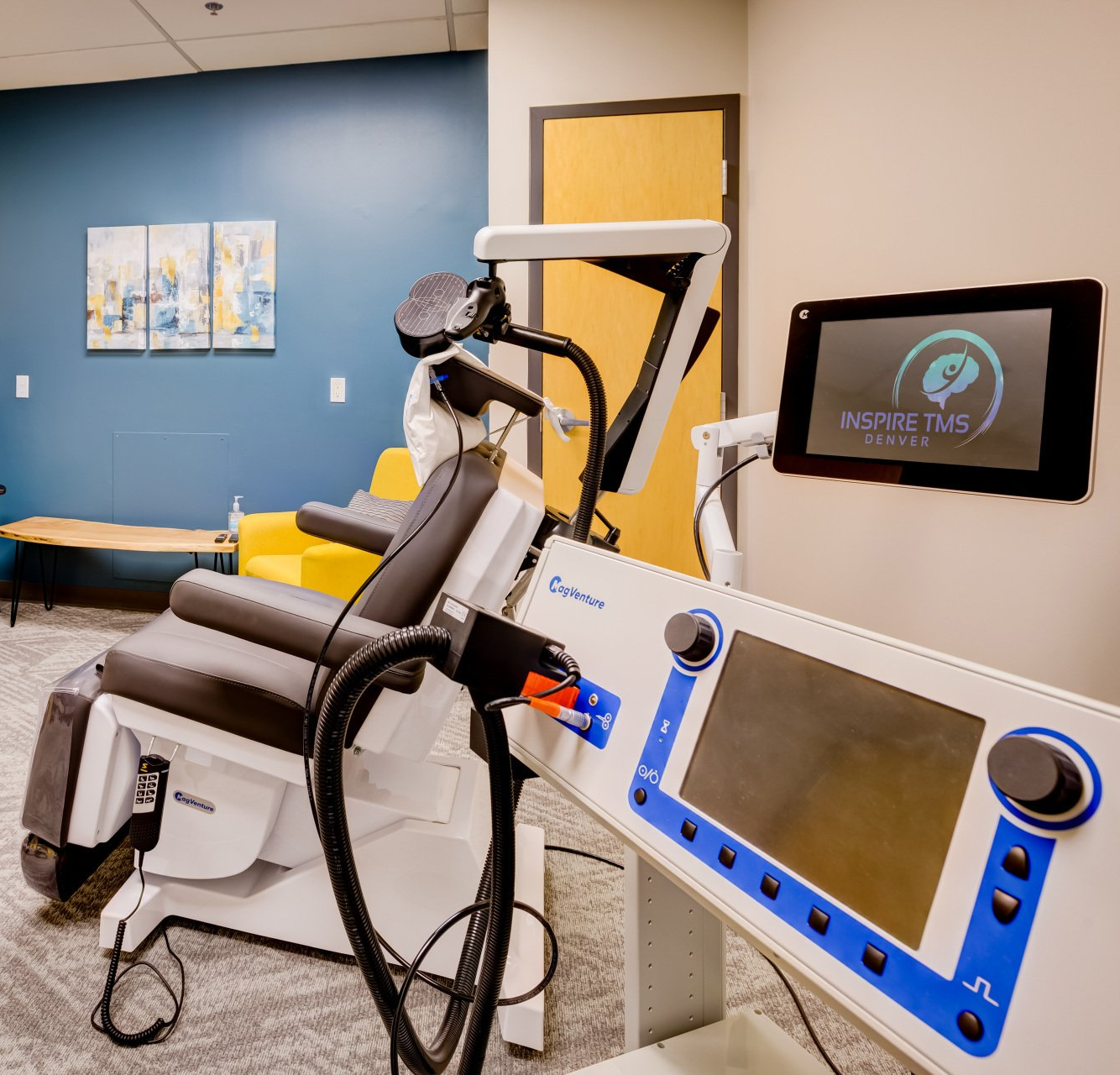
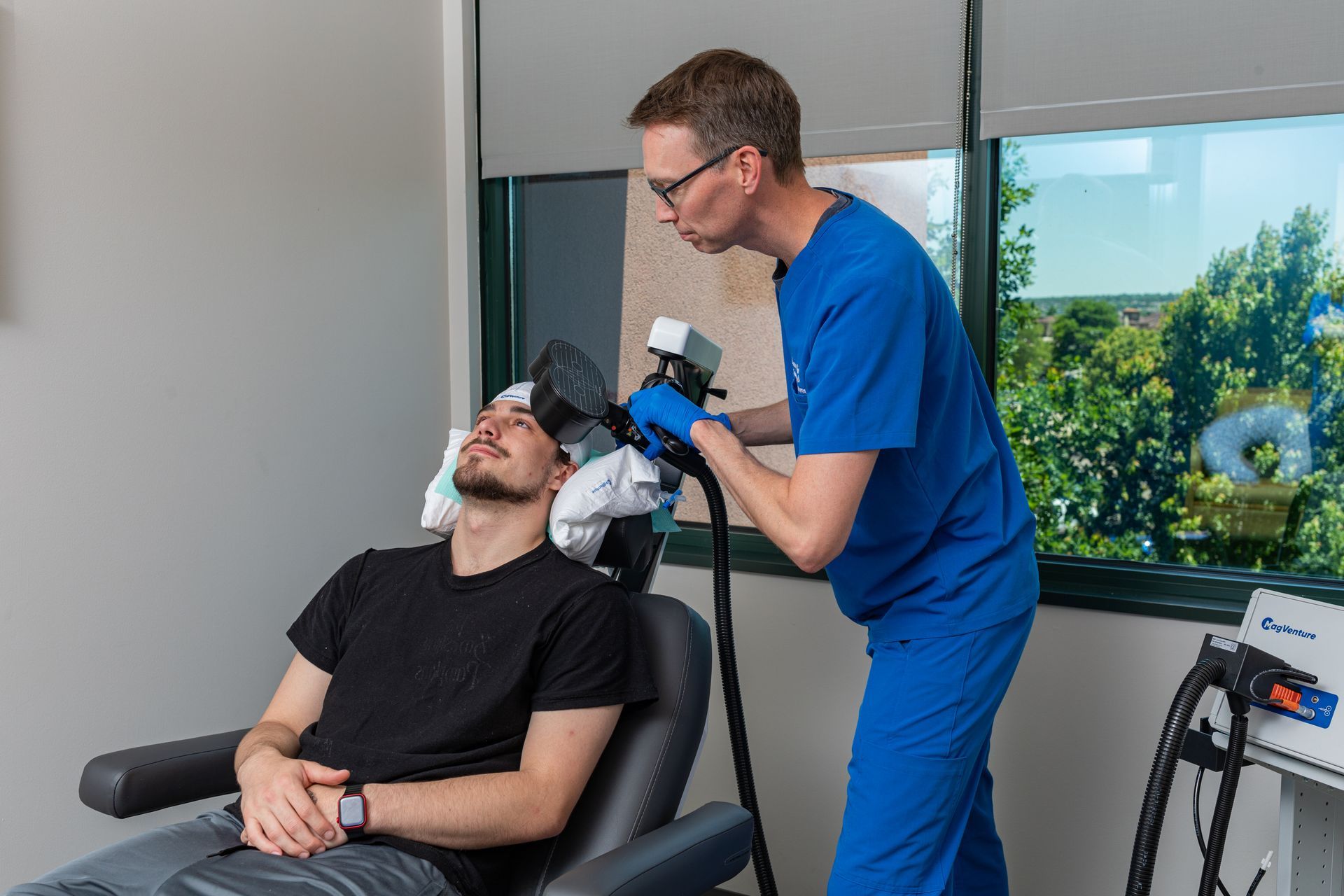
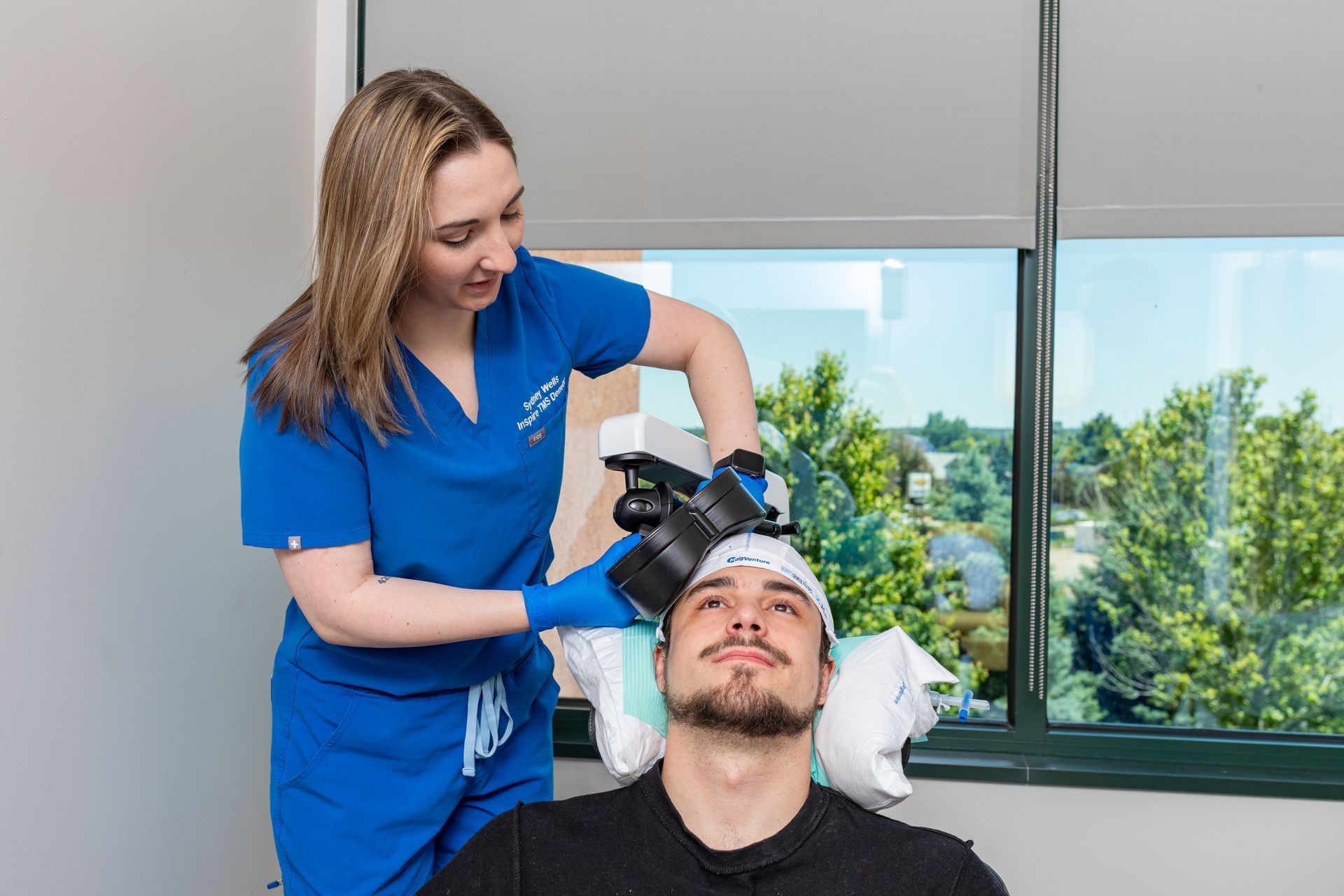
TMS Devices Explained - MagVenture, NeuroStar & Deep TMS

When you’re researching TMS clinics, you’ll see different brand names and device types - MagVenture, NeuroStar, “Deep TMS” (H-coil), and more. That variety can feel confusing, so here’s a plain-language explanation of what the differences mean for you and the smart questions to ask before you book.
The short version
Device choice mostly affects how stimulation is delivered, which influences:
- Which protocols a clinic can offer (standard rTMS, iTBS/Theta Burst, accelerated/One-Day schedules).
- Session length (iTBS sessions are very short; older rTMS sessions are longer).
- Comfort & noise profile (coil shape and pulse characteristics feel different).
- Which brain targets are practical (some coils stimulate deeper or wider networks)?
- Administrative and insurance details (some devices have specific FDA indications or coverage histories).
Importantly, good clinical outcomes depend more on clinician skill, mapping, and monitoring than on brand alone. Device capability matters - but physician-led mapping, correct dosing, and careful follow-up make the biggest difference.
Device types explained (plain language)
Conventional rTMS
- What it does: Delivers focused stimulation to a relatively small cortical area.
- Patient experience: Brief tapping sensation at the skull; sessions take longer than iTBS.
- Why clinics use it: Reliable for many standard depression protocols and widely available.
iTBS (intermittent Theta-Burst Stimulation) capable devices
- What it does: Uses very short bursts of stimulation that produce similar biological effects as standard rTMS but in far less time.
- Patient experience: Sessions can be minutes long instead of 20–30+ minutes.
- Why it matters: Shorter appointments are often better for scheduling and comfort; many clinics combine iTBS with accelerated schedules.
MagVenture (brand)
- What it is: A widely used manufacturer; some MagVenture systems are commonly used for accelerated/One-Day regimens.
- Why you’ll hear it: Clinics sometimes mention MagVenture when they offer compressed/accelerated protocols because of that device’s capabilities in certain settings.
NeuroStar (brand)
- What it is: A long-standing, widely used TMS platform with established clinical workflows and FDA clearances for depression.
- Why you’ll hear it: NeuroStar has substantial real-world data and brand recognition.
Deep TMS / H-coil (different coil geometry)
- What it does: Designed to stimulate broader or deeper brain regions than a figure-8 coil.
- Patient experience: Similar sensations but designed for different targets; used for certain FDA-cleared indications (including OCD in some systems).
- Why it matters: May be an option when deeper networks are targeted, depending on diagnosis and evidence.

Download Your Roadmap to TMS
Want a clear picture of what to expect? Download the TMS Treatment Roadmap by Sydney
What device doesn’t change (and what matters more)
- The device alone does NOT guarantee success. Outcomes depend on clinician expertise, accurate mapping, individualized dosing, ongoing measurement (PHQ-9), and appropriate follow-up - those are the biggest drivers of real results.
- Good clinics document mapping & outcomes. Ask to see how they measure success and adapt care - that’s more important than the logo on the machine.
Practical things, device choice can affect patients
- Appointment length: iTBS = very short sessions; other protocols = longer sessions.
- Accelerated options: Some devices/protocols make compressed One-Day or multi-session/day formats more practical. Clinics offering accelerated care will tell you which devices they use.
- Comfort: Coil shape, pulse pattern, and machine noise can change the sensation. If you’re sensitive, ask for descriptions or to hear/see the device ahead of time.
- FDA indications & insurance: Some devices have specific cleared indications (and differing insurance histories) - that can affect coverage for certain diagnoses.
Questions to ask a clinic before you book
Here’s a short checklist you can use on a call or at a consult:
- Which device(s) do you use - brand and model?
- Which protocols do you offer on that device? (standard rTMS, iTBS, accelerated/One-Day, Deep TMS)
- Is this device capable of the accelerated protocol I’m interested in? (if you want One-Day or iTBS)
- What training do your staff and physicians have with this device? (ask for physician oversight)
- How do you map and document coil position and dose? (precision & mapping are essential)
- What should I expect the session to feel like, and how long will it take?
- Are there any device-specific side effects or comfort issues I should know about?
- Does the device have specific FDA indications relevant to my diagnosis, and how does that affect coverage?
- Can I see an example of outcome tracking/reporting for patients treated with this device? (ask about PHQ-9/GAD-7 tracking)
- What happens if the first device/protocol doesn’t work — do you remap or switch approaches? (Good clinics have standard remap/adjust workflows)
A short clinician note on choosing a device vs choosing a clinic
Clinician skill, careful mapping, and outcome tracking make the biggest difference in safety and results. Device capability influences which options are available, but choose a clinic with experienced physicians who document maps, monitor outcomes, and adapt care - that matters far more than a brand name alone.
Does it matter which TMS device a clinic uses?
Yes, but less than you'd think. The device shapes which protocols are available and how sessions feel — but outcomes depend far more on clinician skill, accurate mapping, and follow-up care than on brand name.
What's the difference between Deep TMS and standard TMS?
Standard TMS uses a focused figure-of-eight coil. Deep TMS uses a different coil geometry to stimulate broader or deeper brain regions. Broader isn't automatically better — it can increase side effect risk. Your diagnosis should drive that decision, not marketing.
What is iTBS and why does it matter?
iTBS delivers stimulation in short bursts that produce similar effects to standard rTMS in a fraction of the time — sometimes under 5 minutes per session. It's what makes accelerated and One-Day TMS schedules practical.
Does the TMS device affect insurance coverage?
It can. Some devices have specific FDA indications that influence what insurers will cover. If coverage matters to you, confirm the clinic's device and protocol match your insurer's criteria before you start.

Every Question Answered
Want to know more about TMS? Check out this in-depth guide to TMS therapy with transparent and easy to understand explanations about TMS processes, protocols, and treated conditions.
Latest Posts