A Patient’s One-Day Itinerary - What to Expect from Mapping to Departure
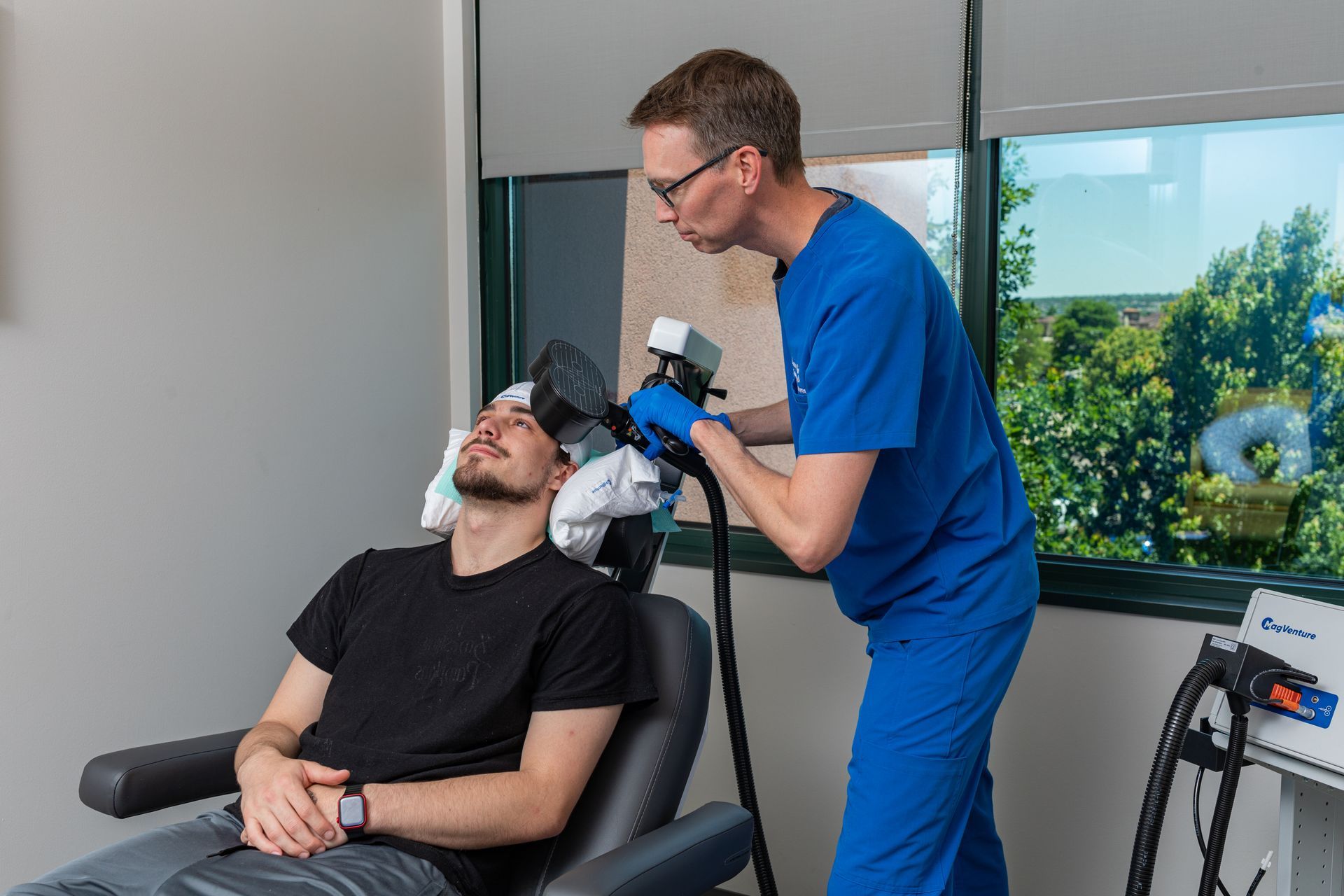
If you’ve chosen a ONE-Day (single-day) TMS course - about 20 short sessions delivered in one (or sometimes two) tightly scheduled days - it helps to know exactly how the day will flow. This patient-facing itinerary shows a typical hour-by-hour timeline, what the clinic does between sessions, what to pack, and simple tips to manage fatigue so your visit is as comfortable and effective as possible.
You’ll arrive for a physician consult and motor-threshold mapping, then remain at the clinic for a block of short stimulation sessions with scheduled comfort breaks and outcome checks; the clinic monitors you closely and provides an end-of-day review and written summary.
Sample hour-by-hour ONE-Day schedule (typical)
08:00 – 09:00 - Arrival, registration & physician consult
- Check in, confirm meds, and medical history.
- Short physician discussion about goals and safety.
- Clinic staff review consent and logistics.
09:00 – 10:00 - Motor-threshold mapping (30–60 min)
- Mapping identifies the stimulation intensity that produces a small motor response and documents coil coordinates.
- Staff records the exact coil position (so every session is reproducible).
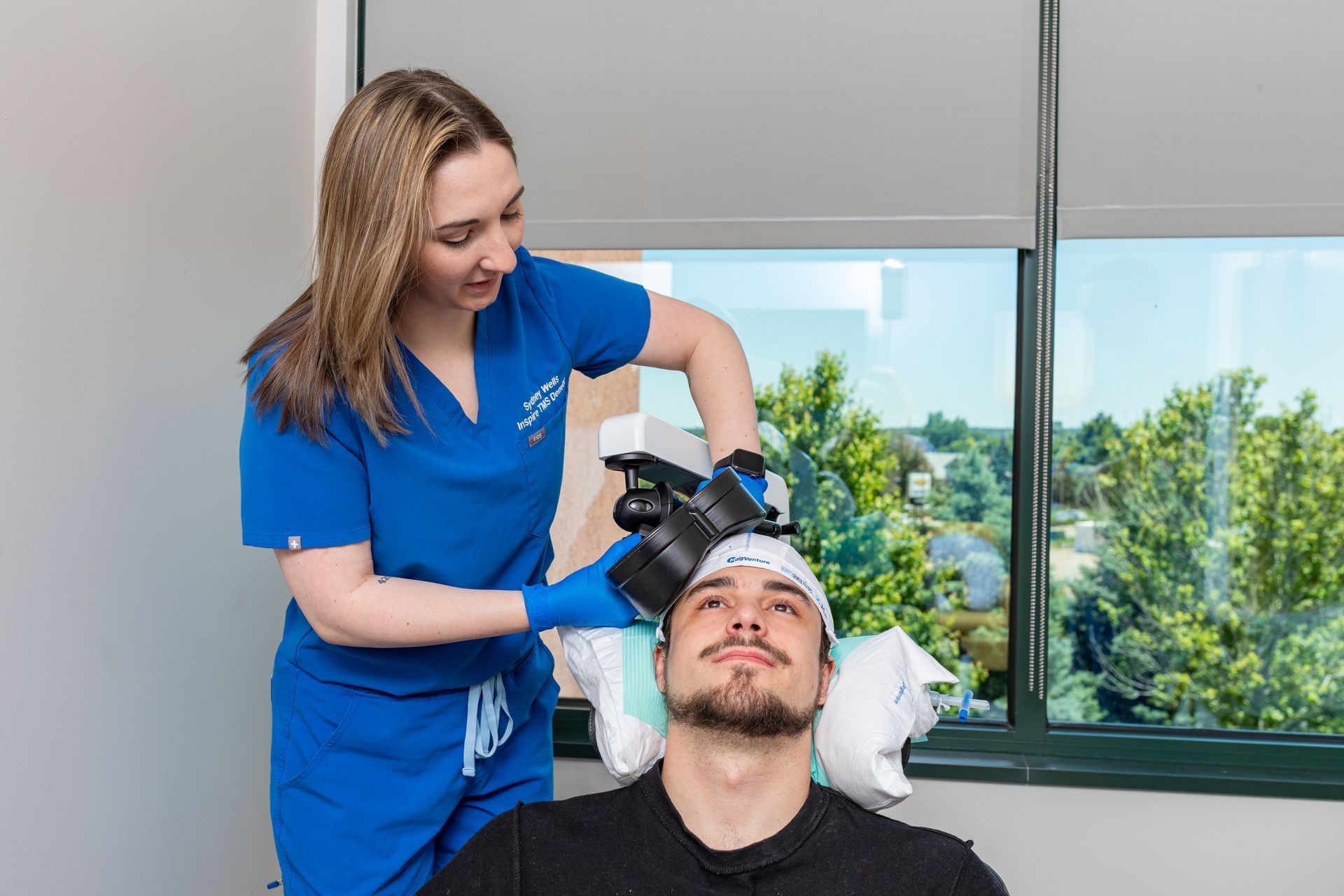
10:00 – 12:30 - Treatment sessions (Block 1: Sessions 1–10)
- Multiple short stimulations (each session minutes long; setup/reset time between sessions).
- Comfort breaks every 2–3 sessions.
- Nursing/tech staff perform quick symptom checks during breaks.
12:30 – 13:30 - Lunch & outcome check
- A longer rest; the clinician may perform a short outcome measure (PHQ-9/GAD-7) or check vitals.
- Time to eat, rest, change clothes if desired, and call for support if needed (ride, family).
13:30 – 17:30 - Treatment sessions (Block 2: Sessions 11–20)
- Continue with scheduled short sessions and short comfort breaks.
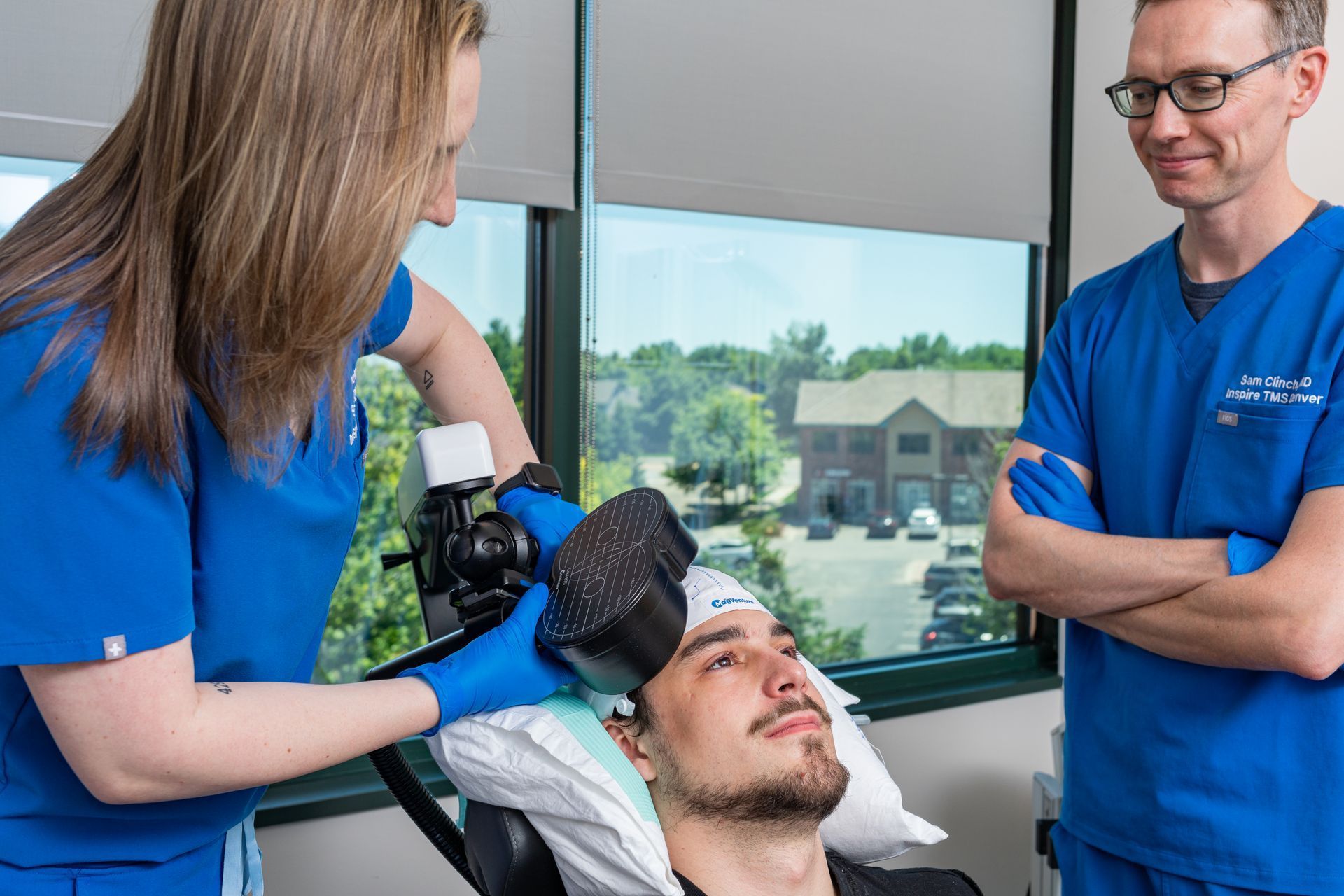
- The team monitors tolerance, symptom scores, and comfort.
- If mapping or pacing adjustments are needed, the physician may make micro-changes.
17:30 – 18:00 - End-of-day review & discharge plan
- Clinician reviews outcome checks, documents the map and dose, and provides a written summary.
- The team discusses next steps: maintenance, boosters, and scheduling follow-up.
Alternative: 1–2 day split - Many patients choose sessions 1–10 on Day 1 and 11–20 on Day 2 to reduce fatigue. The clinic will recommend this based on your history and tolerance.
What the clinic does between sessions
While you rest, the team is working clinically - not just waiting.
- Symptom & safety checks: Quick verbal checks, pain comfort ratings, and short outcome items as needed.
- Documentation: Techs log session parameters, coil coordinates, and any micro-adjustments.
- Titration & micro-adjustments: If a patient reports discomfort or weak responses, the physician may test slight positional or intensity changes.
- Outcome monitoring: We compare brief score snapshots to baseline to spot early plateau and decide if remapping or pacing changes are required.
- Support & comfort: Staff provide water, snacks, and a quiet place to rest. They also address anxiety, nausea, or headache immediately.

Download Your Roadmap to TMS
Want a clear picture of what to expect? Download the TMS Treatment Roadmap by Sydney
Fatigue management - simple, effective tips
ONE-Day is intensive; fatigue is common but manageable.
- Pace your energy: Bring small, portable snacks (nuts, granola bars) and sip water regularly.
- Rest during breaks: Close your eyes, practice deep breathing, or do a short guided relaxation between blocks.
- Avoid heavy meals during treatment: Have a balanced lunch (protein + carbs) but avoid very heavy or greasy foods that increase tiredness.
- Sleep & medication: Keep your usual sleep and medication routine unless the clinic gives other instructions. Insufficient sleep blunts response.
- Accept the need for rest: Plan a low-key activity for the evening, and avoid making critical decisions or long drives if you feel drowsy.
Packing checklist
- Photo ID & insurance card
- Complete medication list (names, doses, last fill times) — critical
- Comfortable clothing and layers (rooms can be cool)
- Phone/tablet + charger and headphones
- Snacks, water bottle, and any preferred beverages
- A book or tablet for quiet breaks
- Emergency contact/ride info (in case you prefer not to drive home)
Practical notes & common patient questions
- Can I drive home? Most patients do, but if you feel fatigued, arrange a ride.
- How long is the clinic stay? Plan for 9–11 hours for a full single-day plan; split days reduce daily time.
- What if I need a remap that day? The physician can remap or adjust pacing if early sessions suggest a micro-change is needed.
How long should I plan for the day?
Expect 9–11 hours for a full ONE-Day visit (mapping + 20 sessions); split 1–2 day visits shorten daily time.
Will I get a written summary?
Yes. You’ll receive a clinician-authored summary of mapping, session details, and next steps for follow-up.
What happens if I don’t tolerate the day?
The team will slow the pace, adjust intensity, remap if needed, or offer a split-day option - patient comfort and safety come first.

Every Question Answered
Want to know more about TMS? Check out this in-depth guide to TMS therapy with transparent and easy to understand explanations about TMS processes, protocols, and treated conditions.
Latest Posts