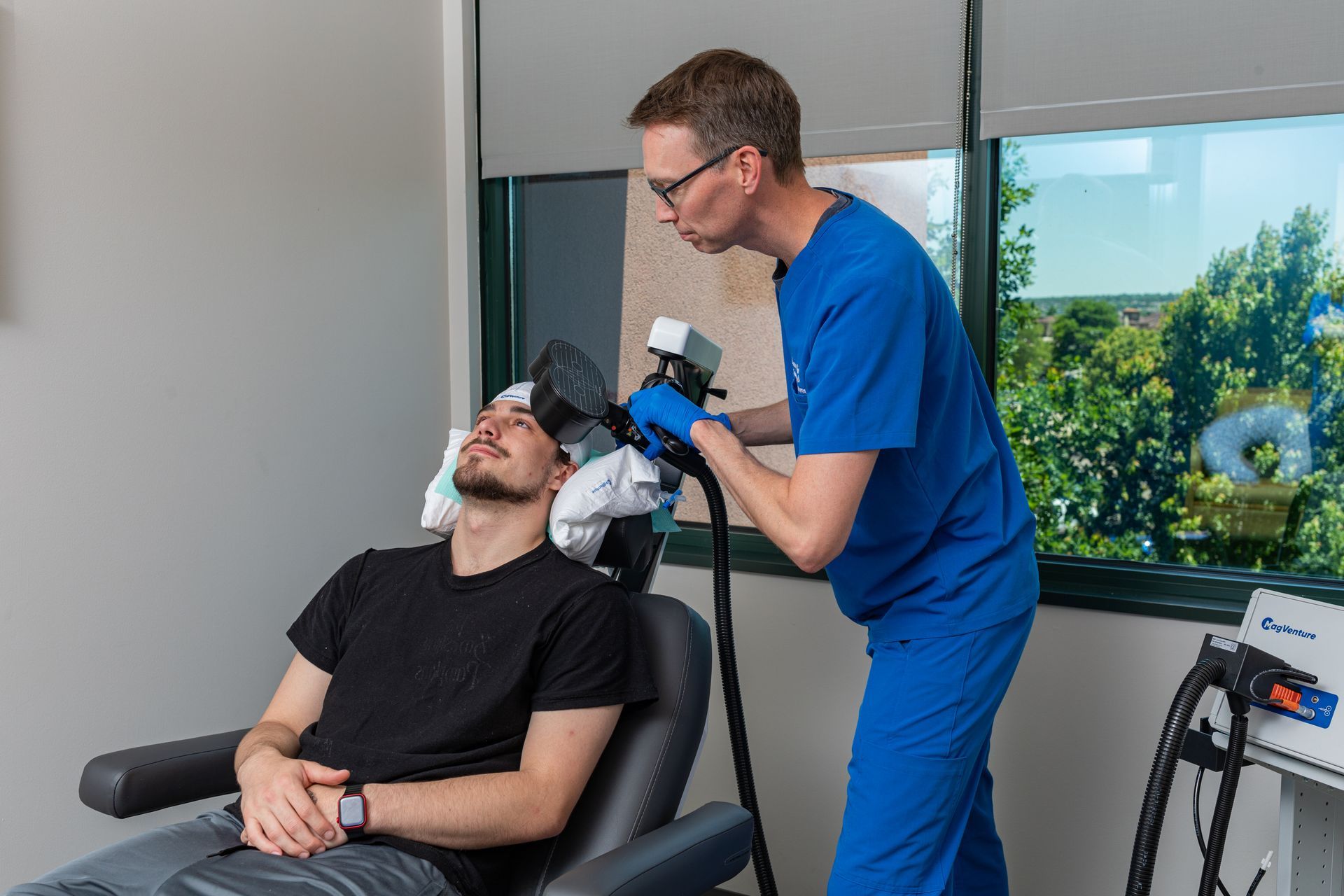
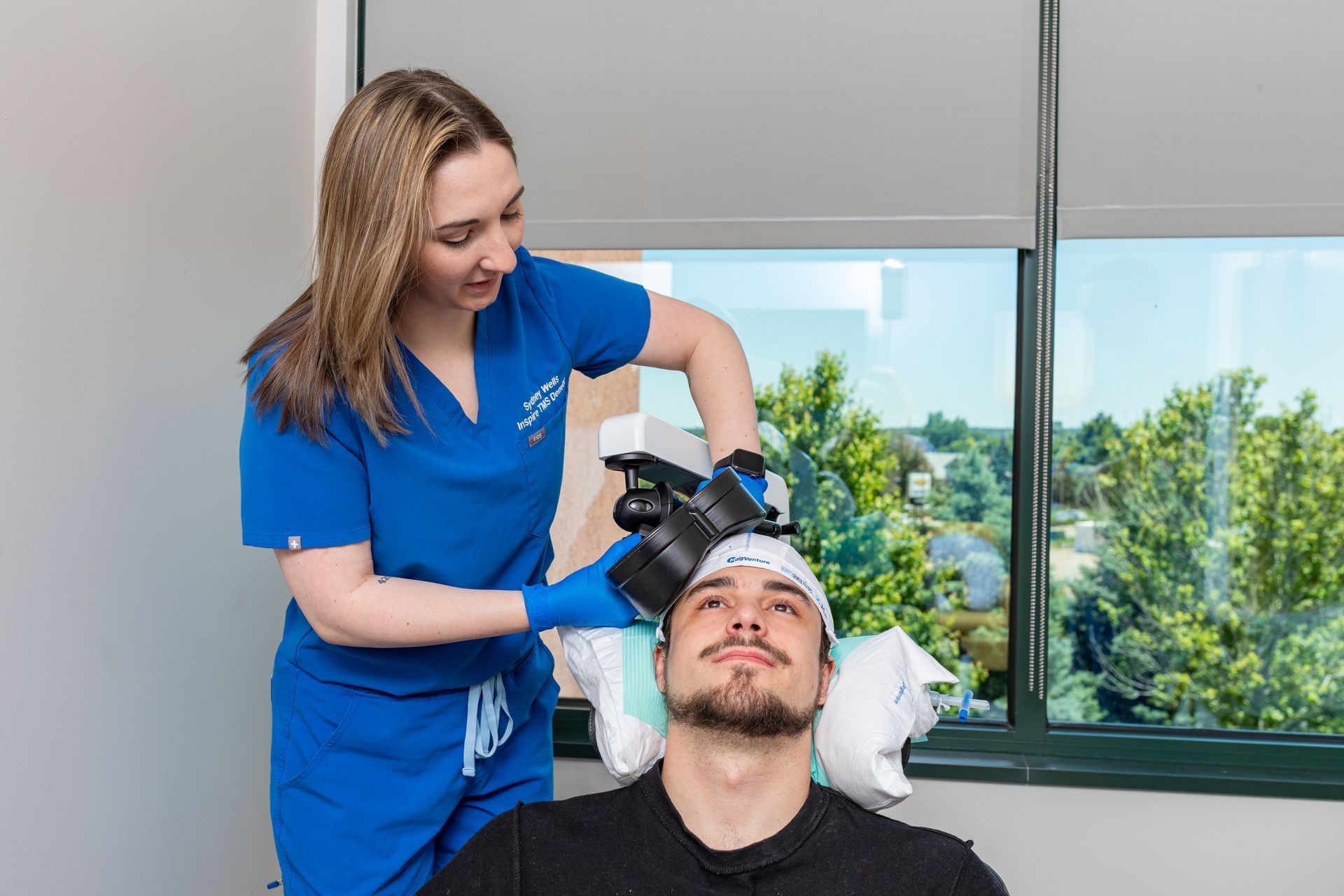
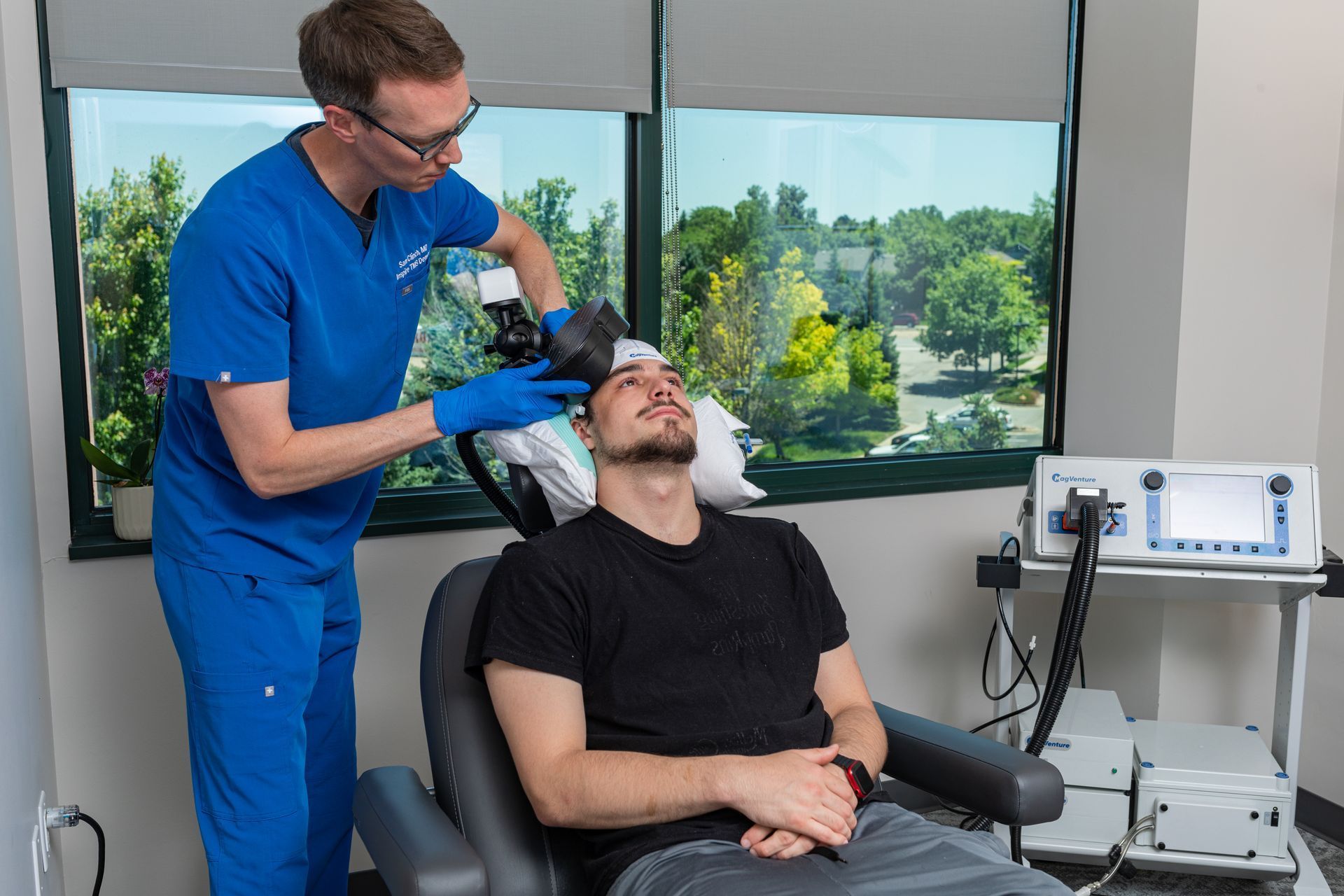
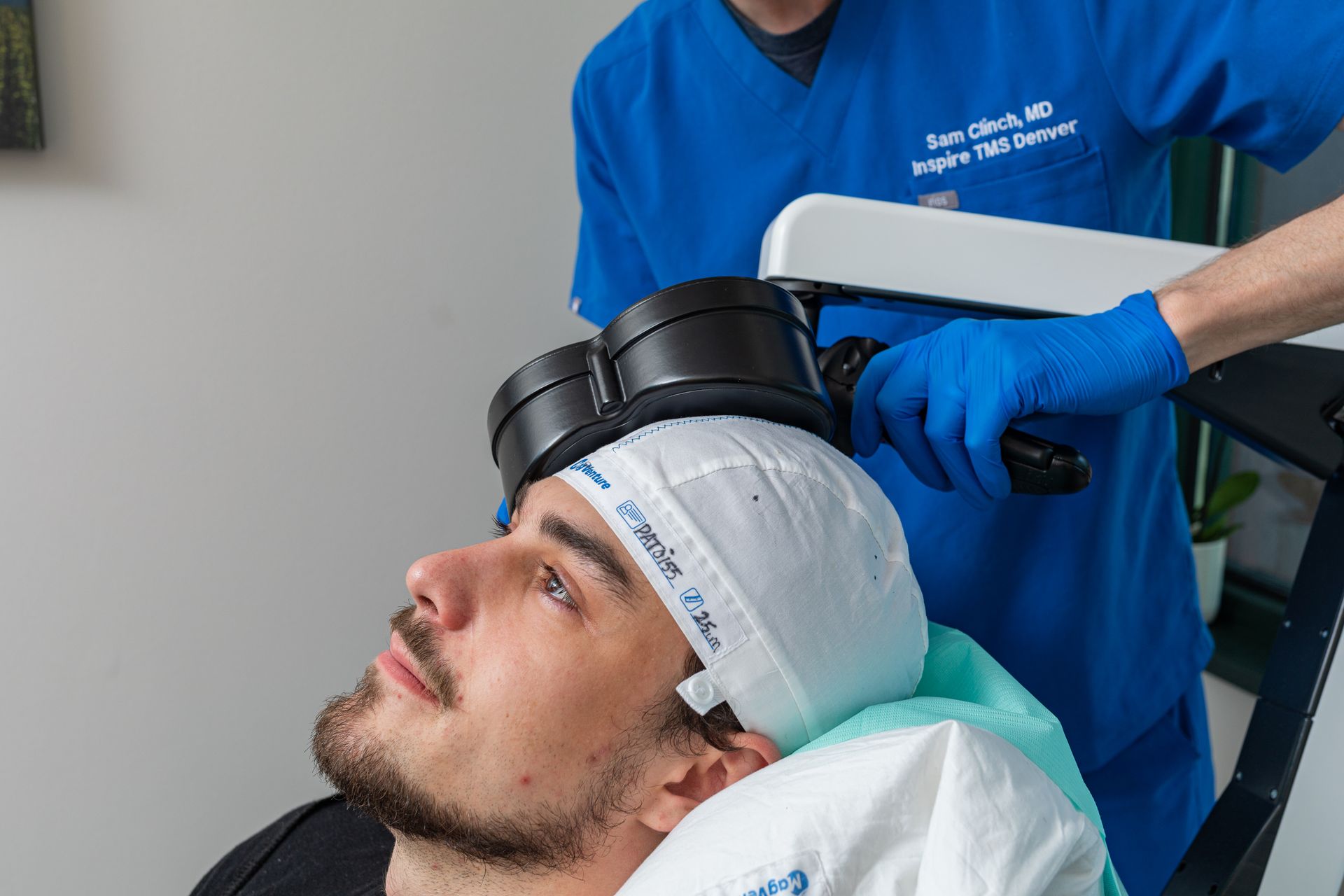
The First 90 Days After TMS: Maintenance, Boosters & What Clinicians Watch For
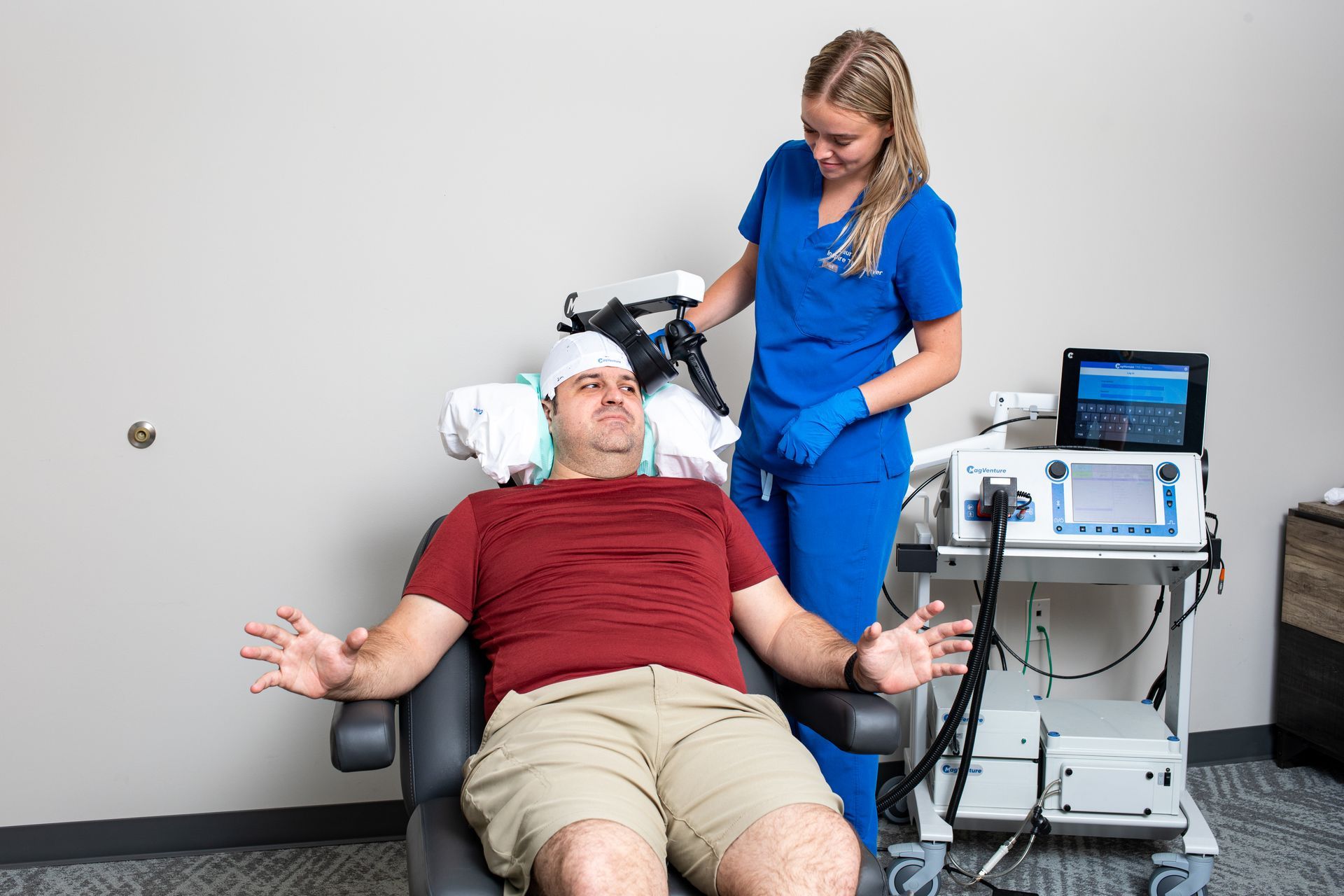
The period following completion of an initial TMS course is critical. At Inspire TMS Denver, we think of the first 90 days as the window when early gains are consolidated, problems are caught early, and long-term plans (maintenance or boosters) are agreed upon. This practical roadmap explains what clinicians monitor, when a booster or maintenance plan is recommended, and what patients can do to protect and extend benefit.
Why the first 90 days matter
TMS causes brain-level changes that unfold over weeks. Some people improve quickly and continue to get better; others show delayed responses or need a small clinical adjustment to translate early signals into durable benefit. The first 90 days are when clinicians can:
- Detect early response vs plateau
- Make targeted adjustments (remap, pacing, or protocol change)
- Decide whether boosters or a maintenance schedule will help sustain gains.
A proactive, measured approach during this window reduces the chance that patients drift away from care when benefit is still within reach.
What clinicians routinely measure and why
At Inspire, we rely on objective signals plus clinical judgment. The core things we track are:
1. Standard outcome scores (weekly → monthly)
PHQ-9 for depression, GAD-7 for anxiety, and other condition-specific scales. These reveal numeric trends that often precede clear subjective change. We typically collect baseline scores, then repeat them weekly (early weeks), moving to biweekly/monthly checks as things stabilize.
2. Functional markers
Sleep, work/school performance, social engagement, and daily activities are measured via short checklists. Function often improves alongside symptom scores - sometimes even earlier.
3. Safety & tolerability
4. Medication, sleep, and life events
Changes in meds, poor sleep, or acute stress/medical events strongly affect response and are always reviewed.
5. Treatment adherence & session data
Missed sessions, pacing changes, or protocol deviations are tracked because they affect outcomes.

Download Your Roadmap to TMS
Want a clear picture of what to expect? Download the TMS Treatment Roadmap by Sydney
What clinicians are watching for (clinical triggers)
Based on these measures, clinicians look for specific signals in the first 90 days:
- Promising trajectory: consistent decline in scores (for example, early week-to-week drops). Continue plan; discuss maintenance when gains consolidate.
- Plateau by Week 3: little or no change by week 3 often triggers a remap or pacing/protocol review. This is a routine precision step, not a failure.
- Late improvement: small early change that accelerates after a remap or adjustment - clinicians watch for this pattern before labeling treatment “non-response.”
- Decline or worsening: any worsening scores or severe side effects prompt immediate clinician contact and review.
- Relapse risk indicators: decline in function, sleep loss, medication non-adherence - may prompt a booster plan sooner.
Maintenance, boosters, and rescue plans explained
Maintenance and boosters are terms patients commonly ask about - here’s how we use them.
Booster session (short course)
Short, targeted sessions are given when a patient shows early signs of symptom return or after a longer gap. A booster can be a few sessions over days or one intensive block, depending on need.
Maintenance schedule
Regular, planned sessions (for example, monthly or every 6–8 weeks) aimed at sustaining gains. Not everyone needs maintenance; it’s individualized based on risk of relapse, prior course response, and life circumstances.
Rescue course
A more substantial repeat course for patients who relapse substantially. This is a therapeutic re-induction aimed at restoring benefit.
How we decide
We consider the magnitude of symptom return, speed of decline, functional impact, past response patterns, and patient preference. Scores guide this decision: a meaningful decline from a prior best (for example drop below the earlier response threshold) often prompts action.
Typical timelines & examples
- Week 1–2: Early signals - monitor closely. Mild, expected side effects resolve.
- Week 3: Decision point - plateau often prompts remap/adjustment.
- Week 4: Many responders show clear improvement. Discuss maintenance planning if gains are solid.
- Week 6–12: Consolidation - booster or maintenance decisions are made based on trajectory.
Example:
A patient who improves quickly, achieving a 50% reduction by week 4, may move to a maintenance plan (monthly). Another who plateaus at week 3 might be remapped and, after improvement, receive a short booster at month 2 to consolidate gains.
Insurance & practical considerations
- Coverage for maintenance and boosters varies. Some insurers cover medically necessary repeat or maintenance sessions; others may require authorization.
- We run benefits checks and provide itemized estimates so patients understand likely out-of-pocket costs before agreeing to maintenance or boosters.
- For travelers, we coordinate local follow-up or plan booster visits to minimize disruption.
How patients can help outcomes in the first 90 days
- Keep your appointments and follow the prescribed pacing.
- Track sleep and meds and report changes promptly.
- Complete scheduled outcome checks (PHQ-9/GAD-7) - they directly inform care.
- Communicate early about side effects or life stressors. Early flagging makes interventions easier and more effective.
How long after my initial course would I need a booster?
It depends. We decide based on symptom return and scores; many boosters happen months after initial gains, but we act sooner if early decline appears.
Does needing a booster mean TMS stopped working?
No. Boosters and maintenance are part of long-term management - like follow-up dosing for other medical therapies - and often restore or preserve benefit.
Will my insurance cover maintenance?
Policies vary. We run a benefits check to clarify coverage and provide an itemized estimate before you commit.
How do you choose monthly vs less frequent maintenance?
We individualize based on relapse risk, how durable your initial response was, functional needs and practical factors like travel and coverage.

Every Question Answered
Want to know more about TMS? Check out this in-depth guide to TMS therapy with transparent and easy to understand explanations about TMS processes, protocols, and treated conditions.
Latest Posts