TMS Near Boulder - One-Day & Accelerated Care (Local Guide)

If you live in Boulder or the nearby Front Range and are considering TMS, Inspire TMS Denver in Broomfield is an easy, physician-led option for local care and short-trip accelerated plans. Below you’ll find practical local details - approximate drive times, One-Day logistics, hotel & travel tips, and how to get a no-surprise, itemized estimate for your visit.
Why Boulder residents come to Inspire TMS Denver
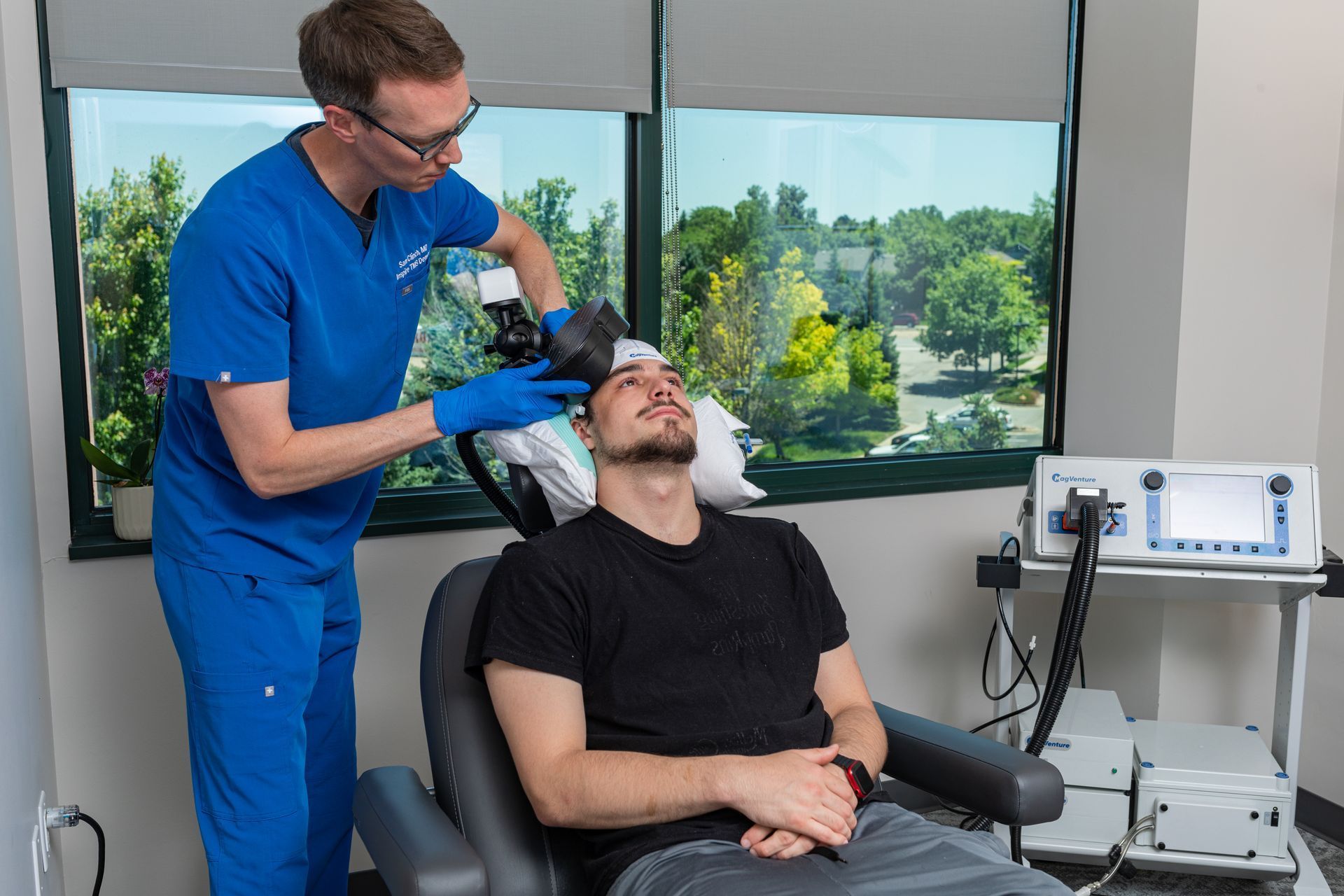
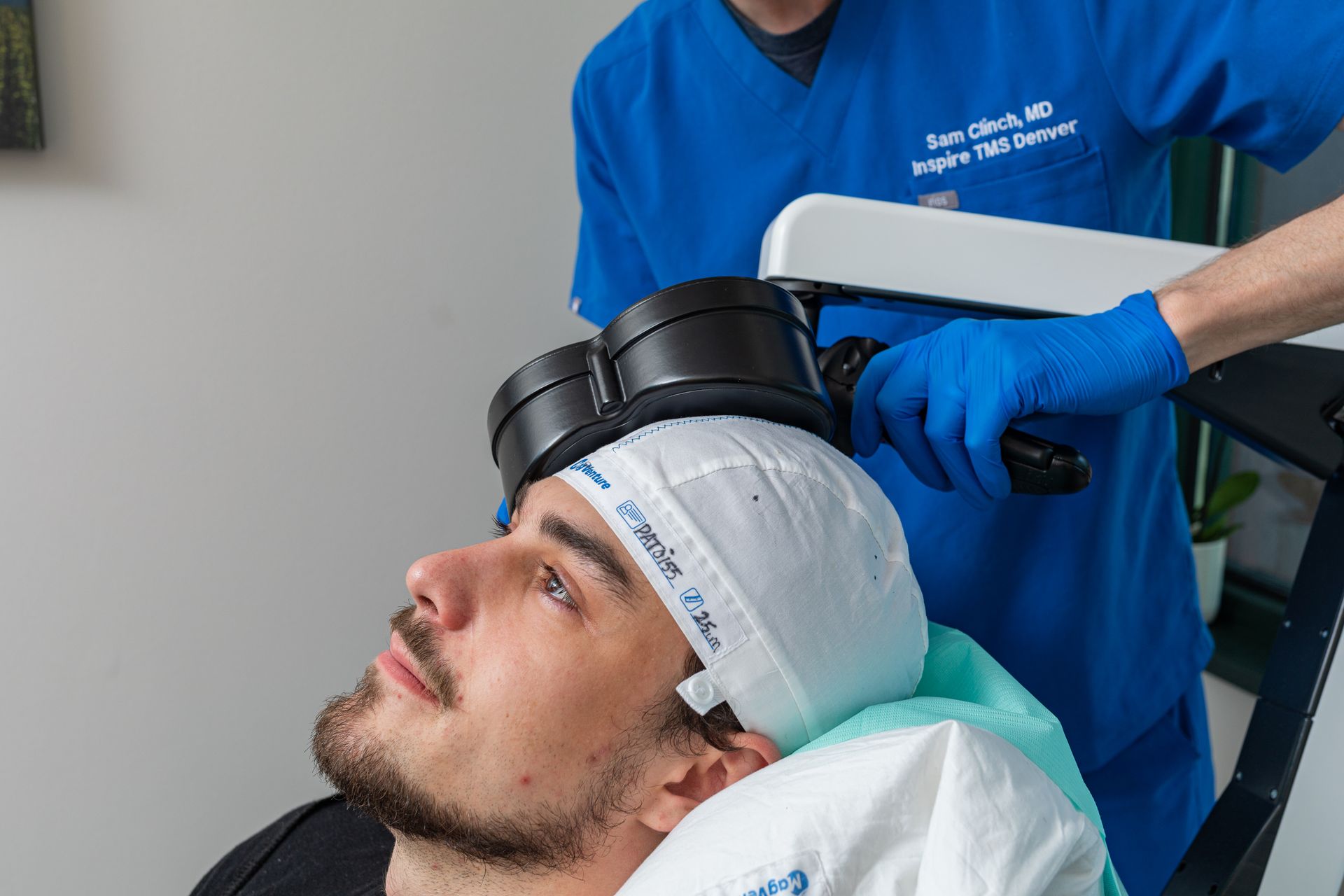
- Physician-led care: Dr. Samuel Clinch personally oversees mapping and accelerated One-Day courses.
- Precision mapping: We perform motor-threshold mapping before any accelerated plan so dose and coil position are individualized.
- One-Day capability: For patients who need fast delivery of the full course, we offer physician-supervised One-Day (20 sessions in 1–2 days) and other accelerated protocols.
- Outcome tracking & follow-up: We monitor PHQ-9/GAD-7 scores and make data-driven adjustments (remap, pacing, boosters) so your trip produces measurable results.

Download Your Roadmap to TMS
Want a clear picture of what to expect? Download the TMS Treatment Roadmap by Sydney
One-Day (Single-Day) logistics for Boulder travelers
Before you travel
- Book a consult & mapping day or a combined mapping + One-Day date. We recommend scheduling the consult and mapping the morning you arrive, unless you want to map on a prior day.
- Send your medication list and any prior TMS records ahead of time - this speeds the consult and safety review.
The typical One-Day flow
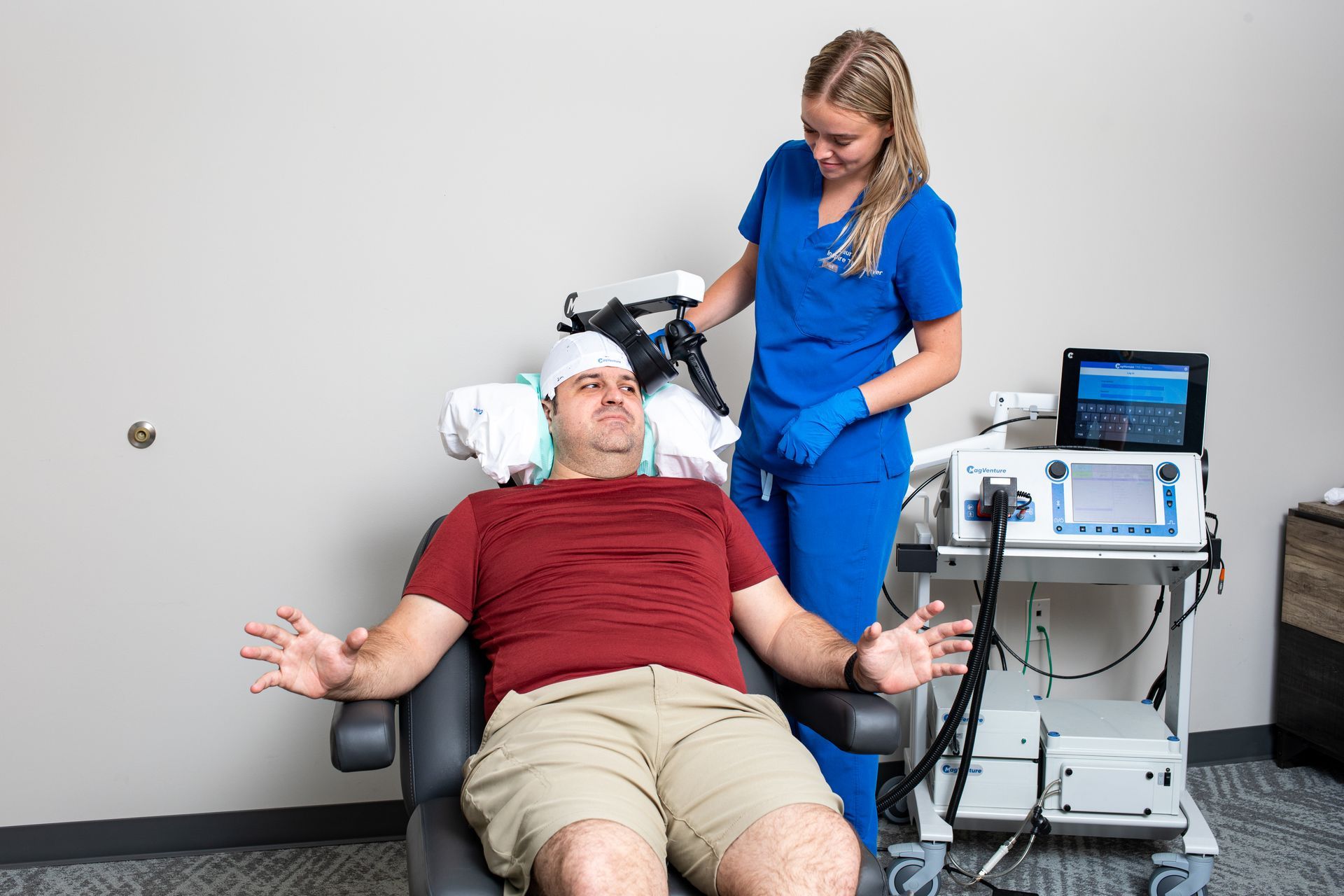
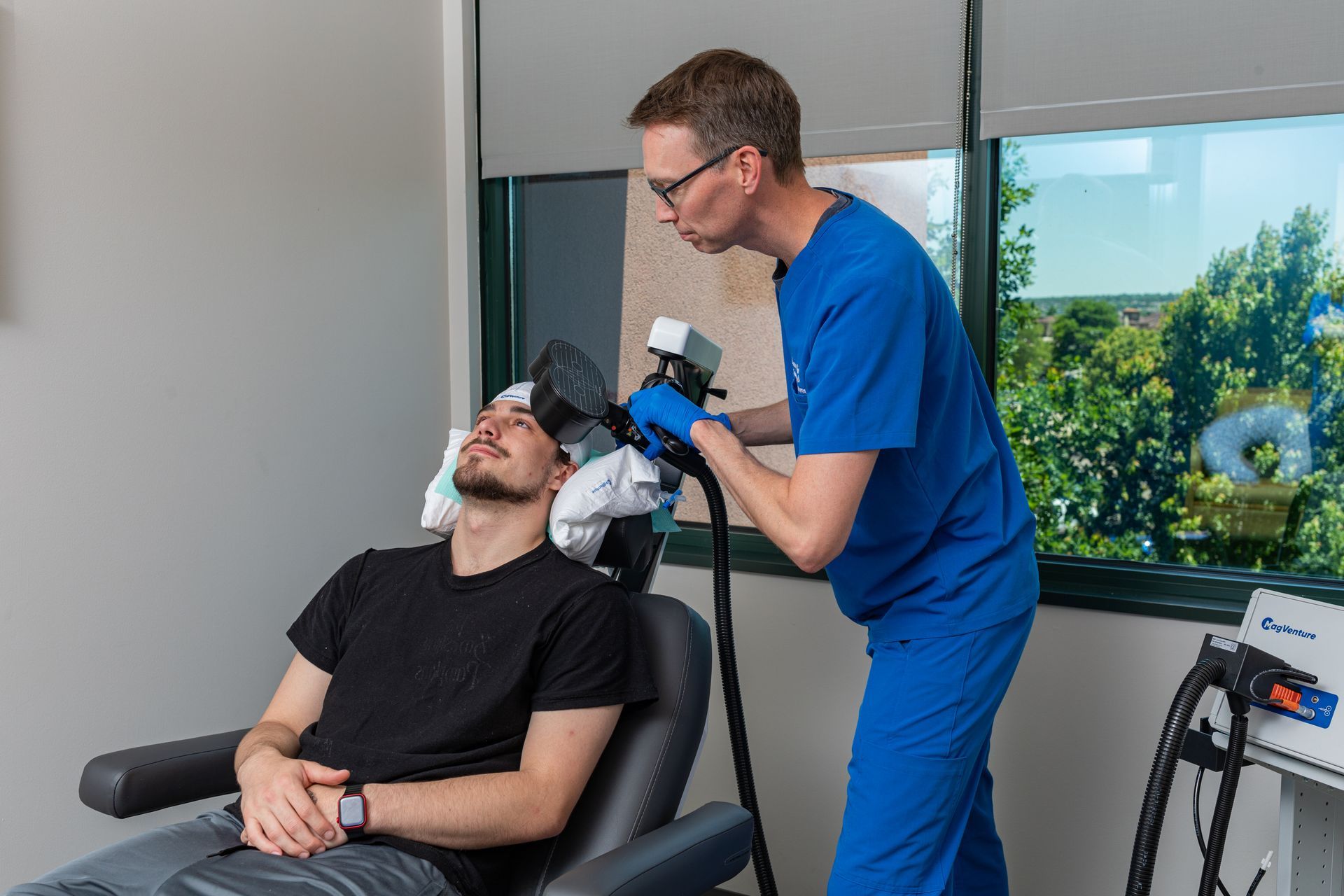
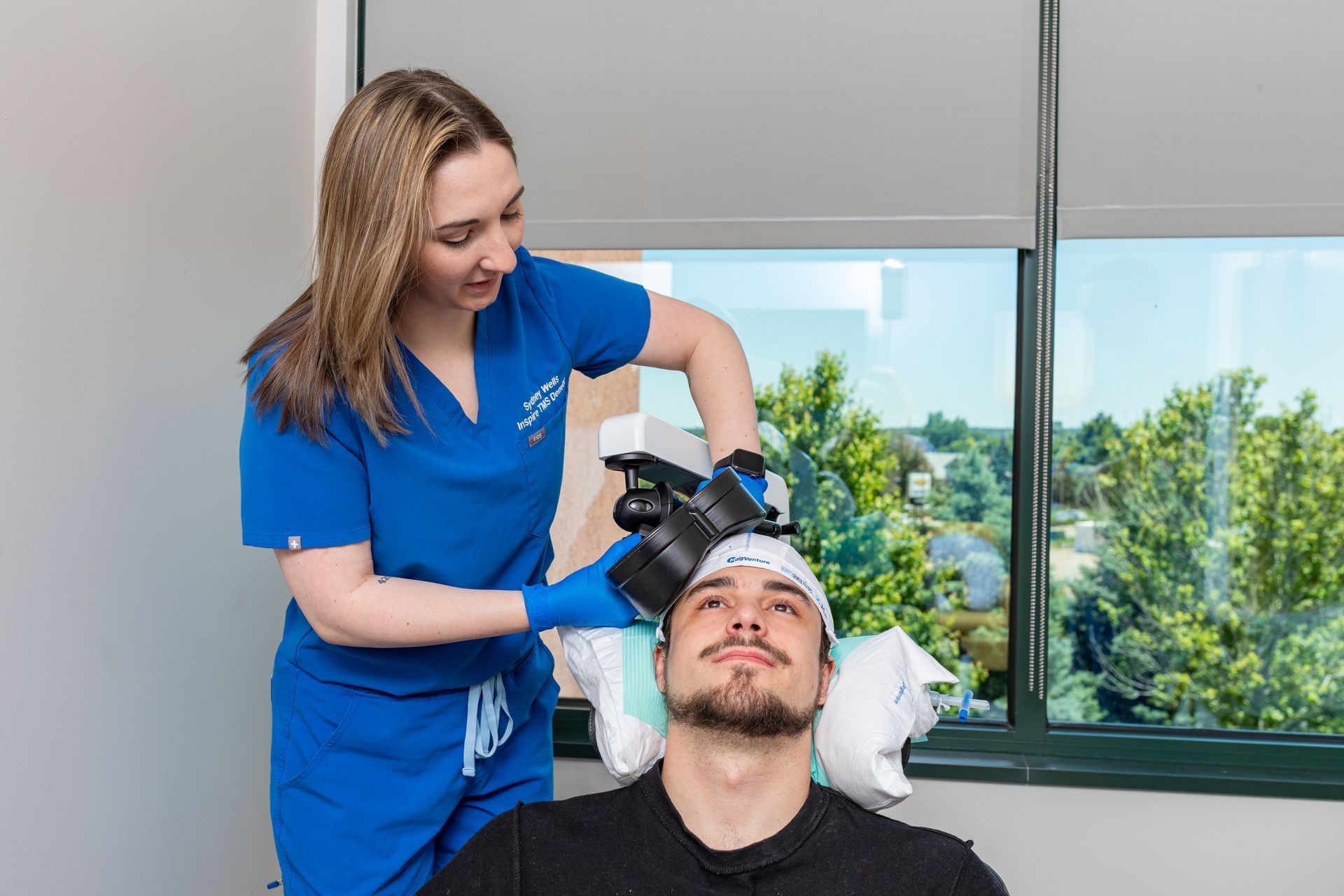
- Arrival & consult + motor-threshold mapping (60 min). Mapping sets your individualized dose and coil coordinates.
- Treatment block(s): Multiple short sessions with scheduled comfort breaks. A true One-Day plan (20 sessions) typically runs 9–11 hours, including mapping, breaks, and an end-of-day review. Some patients prefer a 2-day split for extra recovery.
- End-of-day review & plan: We give you a written summary of the mapping, outcome checks, and next steps (maintenance, boosters, or follow-up).
What to pack & bring
- Photo ID + insurance card
- Complete medication list (names + doses) - critical for safety review
- Comfortable clothes, phone/tablet + charger, headphones, snacks & water
- Plan for rest/transport home - arrange a ride if you expect fatigue
Safety note: Because One-Day is intensive, we monitor symptoms and scores throughout the day and will remap or slow the pace if needed. This is standard physician-led practice, not an emergency.
Hotels & where to stay
Many Boulder patients prefer either staying in Broomfield (near the clinic for an early start) or in Boulder (for sightseeing/family stay). A few practical notes:
- Near the clinic (Broomfield / North Broomfield): Choose hotels near the FlatIron Crossing/Broomfield area for short drives to the clinic and easy parking. These options reduce commute time on treatment day.
- Boulder lodging: If you prefer downtown Boulder (Pearl Street, University Hill), the drive is pleasant and gives you more dining/amenity options - allow 30–40 minutes to reach the clinic.
- Book flexible check-in: If you’re doing One-Day, request early check-in or plan a pre-treatment night so you’re rested for mapping.
Parking & clinic arrival
- Free patient parking is available near the clinic building; follow the arrival instructions we provide in your confirmation.
- Arrive 15 - 30 minutes early to complete any remaining paperwork.
Insurance, cost & itemized estimates
- Coverage varies. Many One-Day 20-session packages are self-pay; some insurers (including Medicare in select circumstances) cover modified accelerated schedules (e.g., two sessions/day).
- No surprises: We run a benefits check and provide a detailed, itemized estimate that shows exactly what your plan would cost out-of-pocket before you commit. This estimate includes consultation, mapping, treatment sessions, monitoring, and follow-up.
- Ask about financing or sliding-scale options if needed - we discuss these transparently.
Can I travel the same day after One-Day?
Most patients can travel the same day, but ONE-DAY is intensive and can cause fatigue - if you expect to be tired, arrange a ride or an overnight stay.
How long will my visit take?
A true One-Day visit (mapping + 20 sessions) is usually 9–11 hours; a 2-day split reduces daily time.
Will my insurance cover this?
Coverage varies - we’ll run a benefits check and give a clear itemized estimate.

Every Question Answered
Want to know more about TMS? Check out this in-depth guide to TMS therapy with transparent and easy to understand explanations about TMS processes, protocols, and treated conditions.
Latest Posts