Returning to Work After TMS: Employment, Accommodations & Success Stories
Quick Summary
Transcranial Magnetic Stimulation (TMS) is an outpatient, non-drug treatment for depression and related conditions. Most patients can resume normal activities, including driving, after a session, and many return to work during or after treatment. This guide gives clear timelines for common TMS protocols (standard, accelerated, ONE-D), examples of reasonable workplace accommodations, ready-to-use employer letter templates, anonymized success stories, and a downloadable Employer Packet to simplify communications and approvals.
Key points up front
- Most patients can drive and work after a TMS session. TMS does not require sedation, and patients typically resume normal activities the same day.
- The timing for returning to full duties varies by protocol. Accelerated protocols and ONE-D compress treatment can be completed in days, requiring planning for multi-hour clinic days; standard TMS involves daily visits over 4–8 weeks.
- Reasonable accommodations - flexible scheduling, remote work, or phased return - usually allow employees to complete TMS while maintaining employment.
- Communication and documentation (a short clinician note, expected schedule, and estimated downtime) speed approvals and reduce stress.
Basic facts employers & HR should know
What TMS is
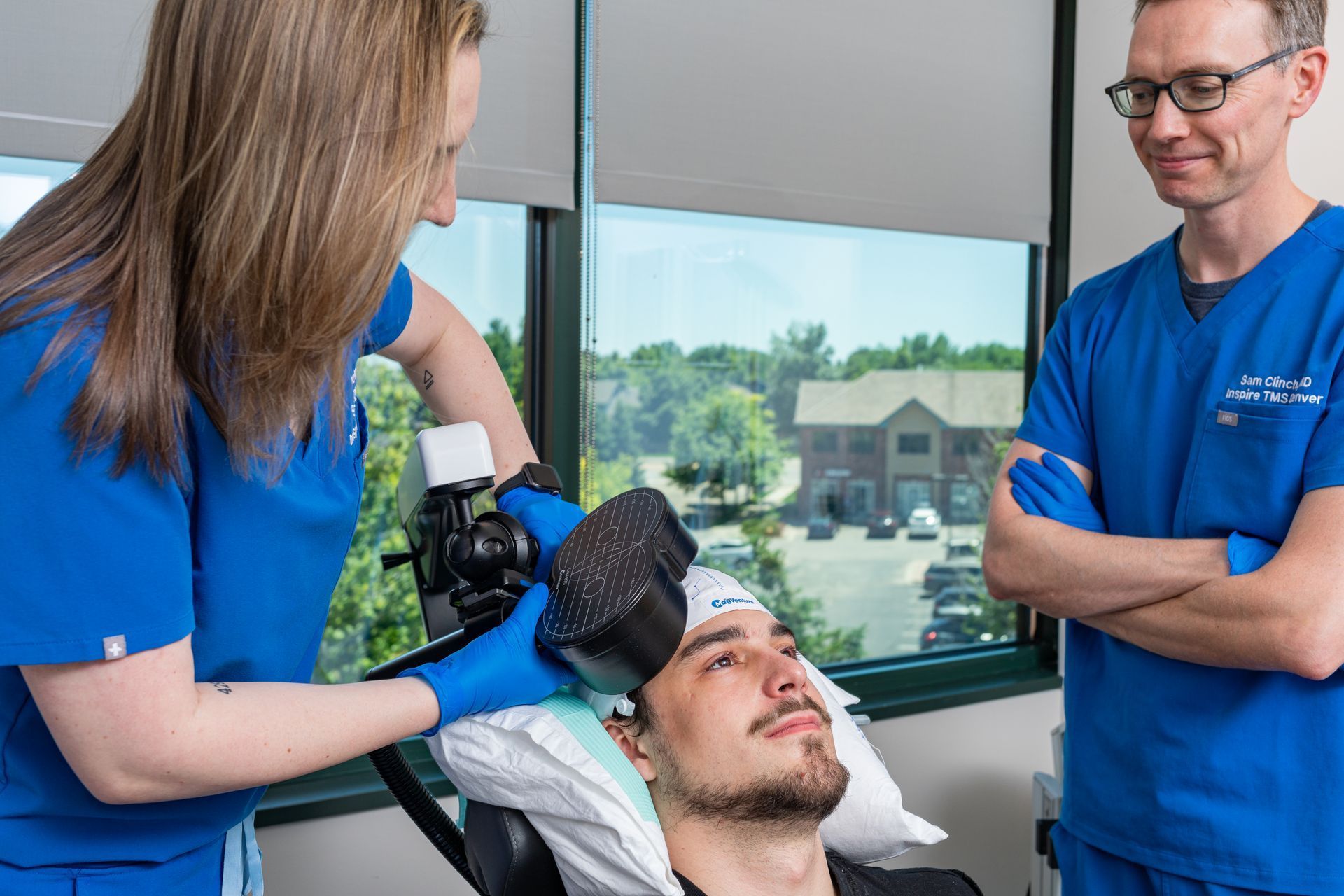
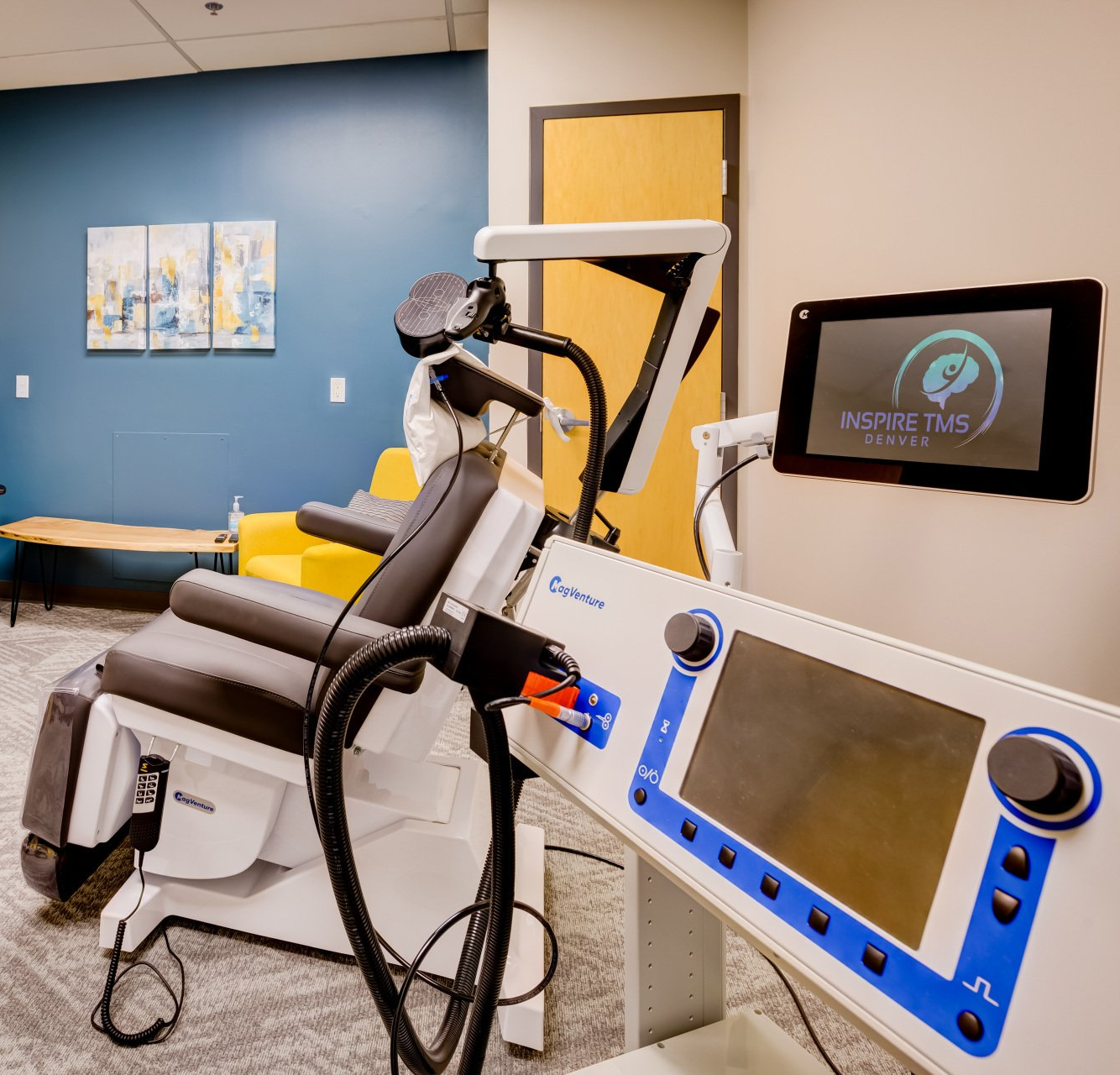
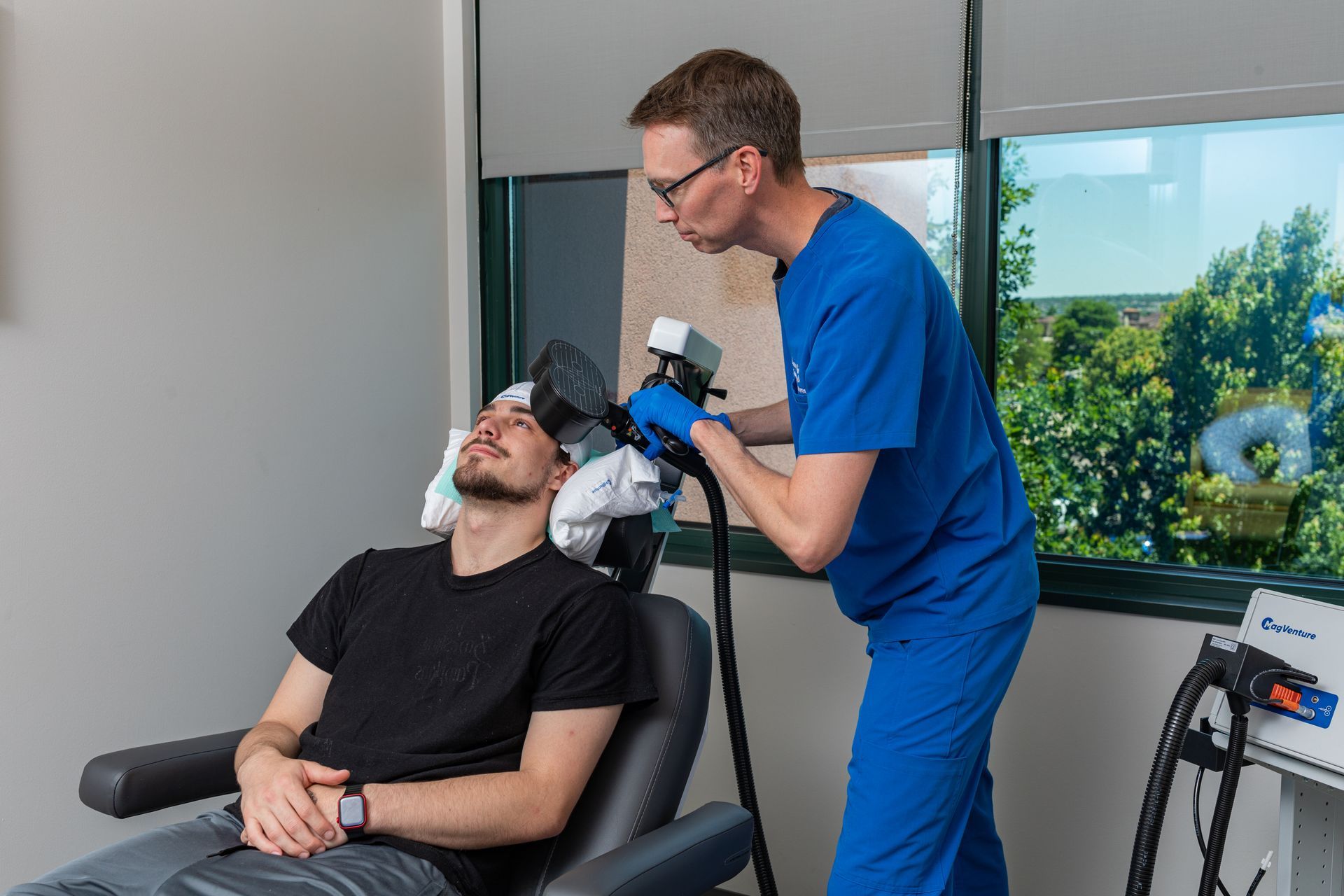
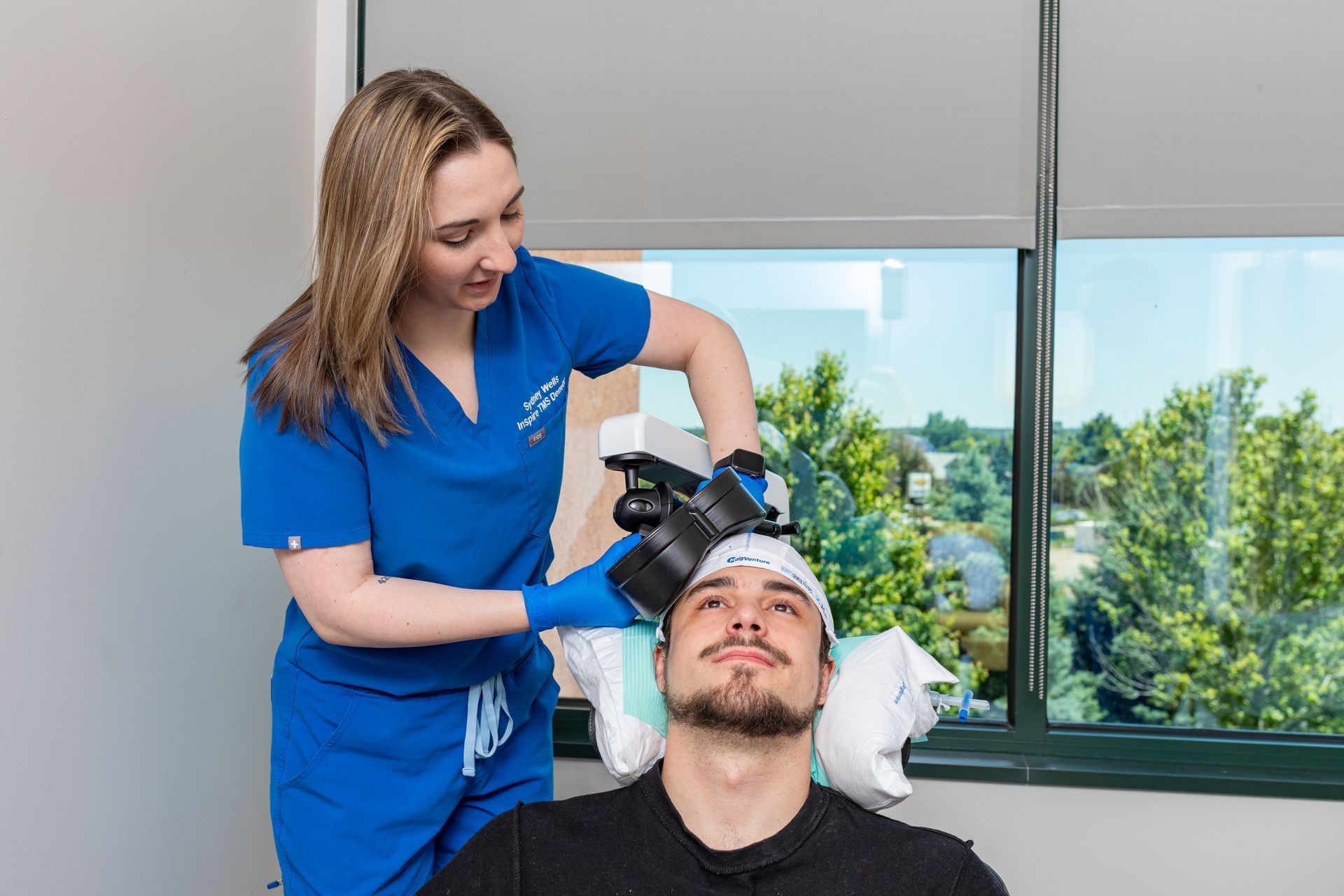
TMS uses magnetic pulses to stimulate targeted brain areas involved in mood. It’s non-invasive, done while the patient is awake, and - unlike ketamine or Spravato® - does not require post-treatment observation that prohibits driving. TMS is performed in an outpatient clinic with physician oversight and safety screening.
Safety & suitability
Clinics screen for
seizure history, implanted metal, and medication interactions before starting mapping and treatment. Mapping is used to personalize stimulation parameters. Employers can rely on a clinician’s assessment and return-to-work guidance.
Typical return-to-work timelines (by protocol)
Use these as guidelines - individual plans should be based on clinician recommendations and job demands.
Standard TMS (typical)
- Schedule: ~1 session/day, Monday–Friday, for 4–6 weeks (some programs 6–8 weeks).
- Daily impact: Sessions last ~20–40 minutes; no sedation. Most patients return to work the same day after a session.
- Work plan: Many patients schedule sessions before or after work, or take short breaks. A phased return (reduced hours first week) is sometimes helpful.
Accelerated TMS (e.g., 50 sessions / 5 days)
- Schedule: Multiple sessions/day (often 8–10/day) over 5 consecutive days. A full clinic day can be long.
- Daily impact: Expect long clinic days; most patients do not work during the treatment week and take time off.
- Work plan: Employers can allow one week of concentrated leave or flexible unpaid leave to accommodate an accelerated week.
ONE-D (Single-Day) or 1–2 day protocols (20 sessions)
- Schedule: 20 iTBS sessions in a single intensive visit or across two days.
- Daily impact: Very condensed; patients usually need the day(s) off for the visit and rest afterward. Employers should treat ONE-D as 1–2 days of medical leave with short-term follow-up.
- Work plan: ONE-D is attractive to travelers and time-limited professionals but requires a short block of leave. (ONE-D is generally self-pay and offered under supervision at select clinics.)

Not Sure If Insurance Covers TMS?
Get a personalized estimate - see if you qualify for insurance and what you’d pay without coverage.
Section 3 - Practical accommodation examples for employers
Below are practical, low-burden accommodations that meet ADA-like fairness for employees undergoing TMS:
Short-term / low-impact accommodations
- Allow flexible start/end times to attend daily sessions (standard protocol).
- Permit remote work for the treatment week for employees with work that can be done remotely.
- Use short-term reduced hours (e.g., 6 hours/day for one week) to help with treatment fatigue.
- Provide protected medical leave for an accelerated week or ONE-D (1–5 business days, depending on the protocol).
Workplace adjustments for safety-sensitive jobs (pilots, ATCs, judges, first responders)
- Require pre-clearance from the employee’s treating physician regarding fitness-for-duty and any medication restrictions.
- Use temporary reassignment to non-safety tasks while undergoing a treatment week.
- Allow graded return to full duties - e.g., light duty for 1–2 weeks, then full duties pending clinician sign-off.
Operational tips
- Request a short clinician note stating: “Patient X is undergoing outpatient TMS. Recommended schedule: [dates]. Expected work impact: [none/minor/leave].” That typically suffices for HR.
- For safety-sensitive roles, require a clinician's fitness statement before returning to full duties.
Employee letter template
Below is a ready-to-use template:
Employee request example for time off (to send to HR/manager)
Subject: Request for Medical Leave - TMS Treatment
Dear [Manager/HR],
I will be undergoing Transcranial Magnetic Stimulation (TMS) treatment for a mental health condition. My plan of care includes [standard daily sessions for 4–6 weeks / one accelerated week (50 sessions over 5 days) / ONE-D: 20 sessions in 1–2 days].
My treating clinic: Inspire TMS Denver - 340 E 1st Ave, Suite 333, Broomfield, CO 80020. They expect the following work impact: [same-day return after sessions / one week leave / 1–2 days leave]. I will provide a clinician note confirming dates and fitness for duty as needed.
Thank you for your support and understanding. Please let me know if you need further documentation.
Sincerely,
[Employee name]

Case studies & success stories (anonymized)
Real, anonymized patient stories illustrate typical return-to-work journeys.
Case study - Compressed week, big gain (Accelerated TMS)
- Work plan: Took one calendar week off, completed the week, returned to reduced hours the following week, and resumed full duties within three weeks of treatment.
- Outcome: Marked reduction in depressive symptoms and improved daily functioning (patient-reported).
Case study - Standard TMS while working
- Background: Patient B received standard TMS (1 session/day over 6 weeks) and scheduled sessions early mornings.
- Work plan: Continued full-time work with minor schedule adjustments for session times.
- Outcome: Able to maintain employment throughout treatment and reported gradual improvement in mood and concentration after 4–6 weeks.
Can an employee drive after a TMS session?
Yes. Standard TMS does not require sedation, and most patients drive and resume normal activities after a session.
Do I need to provide paid leave for TMS?
Not necessarily. Many employees arrange sessions before/after work for standard TMS. Accelerated weeks or ONE-D typically require short leave; employers commonly allow paid or unpaid medical time or flexible scheduling. Discuss options with the employee.
What should a manager ask a clinician?
Ask: “What is the expected work impact? Is a graded return recommended? Are there fitness-for-duty concerns?” A short clinician note is usually sufficient.

Every Question Answered
Want to know more about TMS? Check out this in-depth guide to TMS therapy with transparent and easy to understand explanations about TMS processes, protocols, and treated conditions.
Latest Posts