TMS Ruined My Life, Made Me Worse (Read Before TMS)
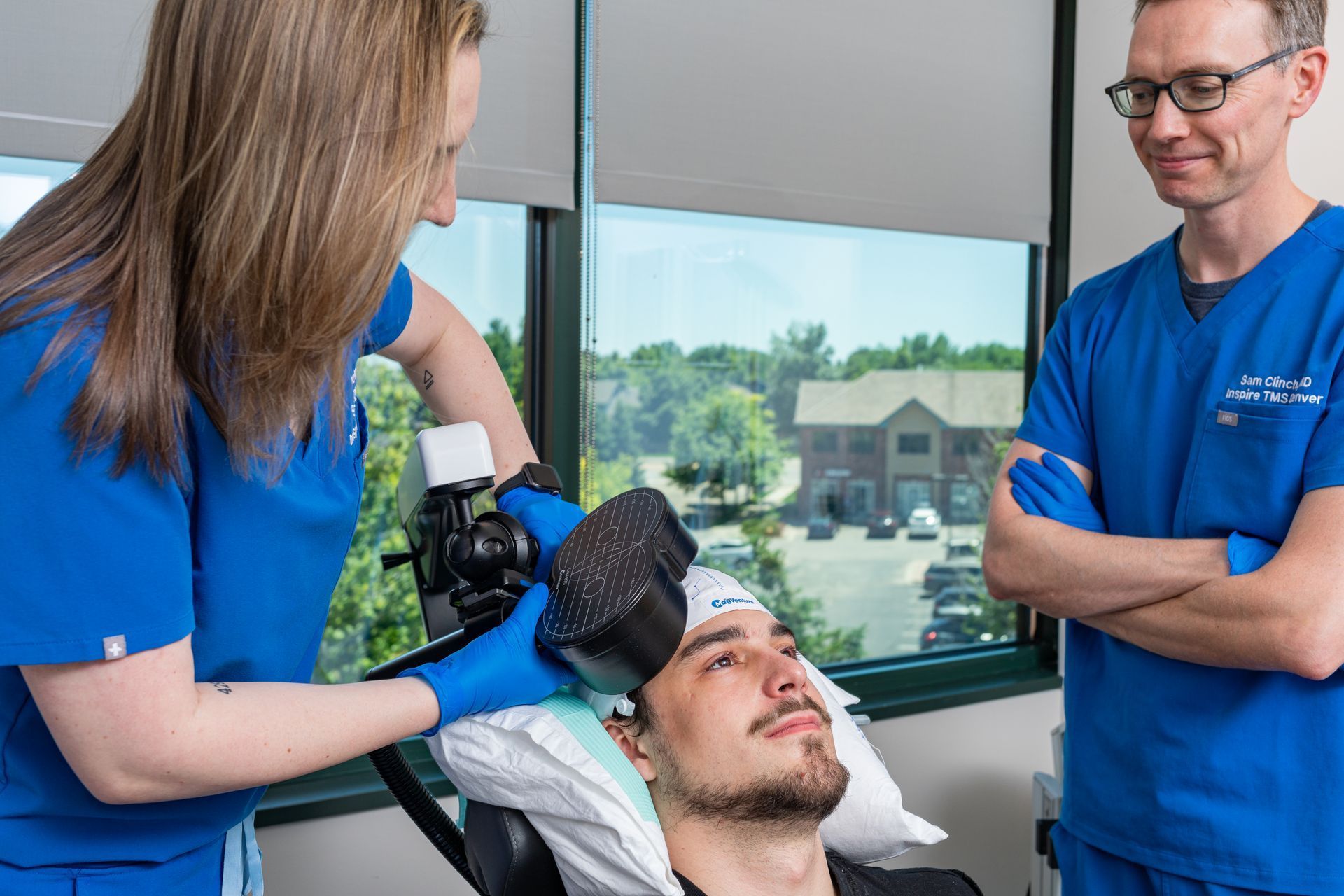
Here’s the truth about Transcranial Magnetic Stimulation
In the past 15 years, TMS therapy has become an increasingly popular treatment for depression and other mental health conditions. As the usage of TMS therapy is on the rise, there has been some increase in negative feedback, particularly on sites such as Reddit. Articles titled “ TMS Ruined My Life ”, and “ TMS Made Me Worse ” have appeared, and cast suspicion on the likelihood of benefiting from TMS treatment. We appreciate that the novel nature of TMS treatment may prompt feelings of apprehension and know that individual results vary with TMS, but in this article, we aim to clarify concerns and provide background on how these reports may be misleading.
First, the evidence that TMS successfully helps a majority of people receiving treatment overcome their depressive symptoms is overwhelming. At Inspire TMS Denver, at least three out of every four patients receiving treatment, report a PHQ-9 score of less than 10 following treatment, which indicates mild to no depressive symptoms. And over 80% of patients report at least a response from TMS treatment (>50% improvement on the PHQ9 score treatment start and finish). Read more:
TMS clinic results for depression →

Not Sure If Insurance Covers TMS?
Get a personalized estimate - see if you qualify for insurance and what you’d pay without coverage.
However, as with any treatment, some patients will not experience relief from TMS therapy. And even some may feel that their symptoms have worsened with treatment. We have stopped treatment for a small number of individuals (approximately 1%) that report intolerable side effects or expressed concerns that treatment was making them feel worse. With cessation of treatment, however, these concerns were resolved. There is always the possibility that treatment may not be delivered appropriately (we specialize in TMS at our clinic and are confident in the treatments we deliver) or that an individual’s condition may have worsened secondary to other factors unrelated to TMS. Acknowledging this occurrence and recognizing that a small percentage may not benefit or may experience rare short term side effects is important to consider. To date, however, there are no studies indicating short or long term safety concerns with TMS treatment. The largest risk with TMS is seizure and this is on the order of 1 in 60,000 treatments. Seizures have not continued beyond treatment or resulted in any additional adverse events. We have not experienced a seizure in our clinic to date and know how to respond should such an event occur. Read more:
TMS therapy pros and cons→
What Is the TMS ‘Dip’
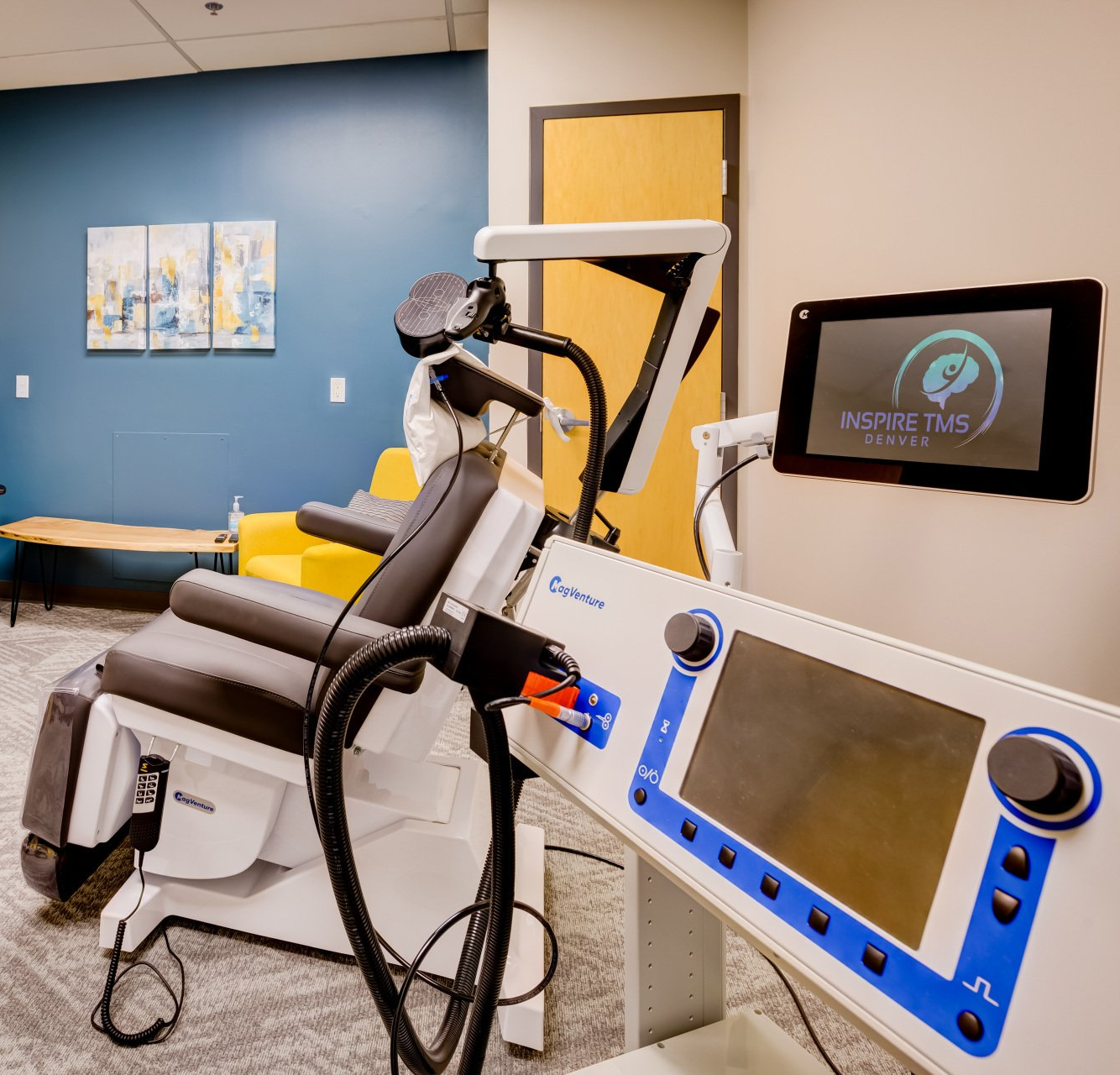
At Inspire TMS Denver, we take pride in providing a therapy option with high success rates and mild, if any, side effects. The most common side effects reported are short-lived headaches and scalp sensitivity where the TMS device delivers magnetic pulses on the patient's head. We have only had one patient stop treatment due to any side effects to date.
For some patients, however, there is also a period in which their depressive or anxiety symptoms may temporarily worsen. This is known as the TMS ‘dip’, and we believe it occurs as a result of fluctuations in brain activity induced by TMS. It is typically observed halfway through the protocol, but can occur at any time. During TMS, neurons in your brain are disrupted as a result of electromagnetic pulses, which can either excite or inhibit brain cell activity. Whilst your brain adjusts to the changes it is undergoing, some patients report short episodes of worsening of symptoms. It is important to note that this exacerbation is temporary, and after additional treatment, a relief in symptoms is observed. If worsening of symptoms occurs earlier in treatment or is persisting, however, it may warrant stopping treatment.
Possible solutions to the TMS ‘dip’ - Maintenance TMS Therapy or Addressing a Misdiagnosis
Each patient will have individual needs, meaning the standard 30 sessions of TMS therapy may not be enough for some people. If, after the protocol has finished, your depressive symptoms have not improved in a way that you are satisfied with, you may require additional sessions of TMS. If you experience positive results with TMS but the benefits do not last, you may need additional sessions to maintain response. This is known as rescue TMS or TMS maintenance, and you should discuss this option with your TMS provider. We offer treatment extension, rescue, and maintenance TMS at Inspire TMS Denver when indicated. If unable to get insurance to cover a repeat course of TMS, we offer these sessions at a discounted rate, or even some treatments free of charge based on financial hardship.
Another possibility for experiencing worsening symptoms following TMS would be a misdiagnosis. Occasionally patients are misdiagnosed and/or have comorbid disorders that may manifest or overlap with depressive symptoms. In these cases, TMS treatment may not affect the brain as expected in typical cases of major depression and the same benefits may not be observed.
TMS is FDA-approved for Major Depression and OCD and has yet to be approved for other mental health disorders. Therefore, re-assessing treatment options if a misdiagnosis occurs is crucial.
Finally, as noted above, symptoms of Major Depression and other psychiatric conditions commonly fluctuate over time based on stressors, other medical issues, and many other reasons that can be difficult to pinpoint. It is certainly possible that TMS may have nothing to do with the worsening of symptoms for individuals who have published reports of TMS worsening their condition.
Having discussions with your TMS treatment team will help to track your progress and ensure that you are getting the most out of your treatment.
Can TMS Actually “Make You Worse” - The Bottom Line
Whilst the effects of TMS therapy are overwhelmingly positive, an individual’s response and perception of their treatment is unique and we respect that perspective. To date, less than 2% of patients we have treated with TMS at Inspire TMS Denver have reported a higher score on their depression scale treatment start to finish. Of these, the percentage increase on that depression scale was never more than a 17% change, with most reporting around a 10% worsening of symptoms based on the depression scale - not reaching statistical significance. None of these patients expressed concern that their condition had actually worsened in the long run either; only that treatment had not proven beneficial. There are, likewise, no current studies supporting that TMS therapy worsens symptoms of depression in the long run, provided that patients have been correctly diagnosed and treated. We also have not had any patients contact us following treatment to report any persistent side effects.
Other TMS Guides...
We can certainly appreciate the frustration of not experiencing relief from treatment, but we are confident and trust that TMS is an effective method for treating Major Depression, OCD, and other evidence-based conditions when administered correctly. Although anecdotal and individual reports can be meaningful, we think it is more important to consider empirical evidence and clinical results from credible sources to develop an informed opinion and decision about TMS.
With an over 80% response rate from our own clinical data, we are confident that TMS treatment is a viable, promising option for those suffering from depression, OCD, and other conditions, and especially for those who have experienced difficulties achieving results with other treatments. We are committed to providing exceptional care and creating a safe, relaxing environment for treatment. At Inspire TMS, we are dedicated to continually adapting to new technology and providing advanced mental health treatment to help relieve severe and nuanced conditions. We also offer many options for treatment, including
Accelerated TMS Therapy with Theta Burst Stimulation, which can provide faster and more significant results.
Can TMS therapy make symptoms worse?
While most patients experience symptom improvement, a small percentage may initially feel worse. This can be due to temporary emotional shifts, increased self-awareness, or co-existing conditions. In most cases, these effects are short-lived and resolve with continued treatment and support.
Why do some people feel like TMS “ruined” their life?
This phrase often reflects frustration from unmet expectations or misdiagnosis. TMS is not a cure-all and works best when patients are properly screened, supported, and treated for the right condition. It’s important to work with experienced providers who understand how to personalize care.
Is feeling worse before feeling better normal during TMS?
Yes, some patients experience mood dips, fatigue, or anxiety early on. These responses can be part of the brain's adjustment to stimulation. Most people notice improvements by week 3–4. Open communication with your provider is key.
Is TMS still safe even if I didn’t improve?
Yes, TMS remains a very safe, FDA-approved treatment. A lack of improvement doesn’t indicate harm. Your experience should still be reviewed, and next steps can be guided by your provider - including touch-up treatments or other therapies.
Can TMS trigger mania or hypomania?
In people with bipolar spectrum conditions, any antidepressant intervention (including TMS) can occasionally trigger hypomania or mania. That’s why clinicians screen for bipolar features and monitor mood closely. If mood elevation occurs, your clinician will adjust the plan and coordinate psychiatric care.
What if my clinic delivered TMS incorrectly - does that happen?
Outcomes can be affected by how treatment is delivered. Best practice includes physician oversight, proper motor-threshold mapping, and trained staff. If you suspect your care was substandard, discuss it with your provider and seek a second opinion if needed.
Could my diagnosis be wrong or incomplete - and could that be why TMS didn’t help?
Yes. Comorbid conditions (bipolar disorder, PTSD, personality disorders, medical problems) or an initial misdiagnosis can affect TMS outcomes. If TMS is not helping as expected, a thorough psychiatric re-evaluation is important to ensure the right treatment plan.
How rare / how serious are major TMS risks like seizures?
Major complications are extremely uncommon. The largest reported risk is seizure, estimated on the order of one in tens of thousands of treatments. Clinics screen patients carefully and are trained to respond if a rare serious event occurs.
What is the “TMS dip”?
The “TMS dip” is a temporary worsening of mood or anxiety that some patients experience while the brain is adjusting to stimulation. It commonly appears mid-course and typically improves with continued therapy or minor protocol changes.

Every Question Answered
Want to know more about TMS? Check out this in-depth guide to TMS therapy with transparent and easy to understand explanations about TMS processes, protocols, and treated conditions.
Latest Posts